The causative agent of herpes is one of those viruses that, once introduced into the body, remain in it forever. How can you protect yourself from a dangerous disease? And how to resist infection if infection does occur?
Herpes (from the Greek herpete, meaning “to crawl”) is a widespread disease caused by viruses of the Herpesviridae family, which has about 100 microorganisms and is characterized by a variety of clinical manifestations, usually a chronic course, as well as various routes of transmission of infectious agents. Of the large family of herpes viruses, only 8 cause human diseases.
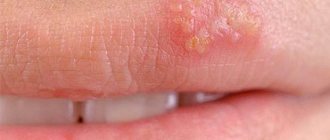
Simple recurrent (recurring) herpes is a disease caused by the herpes simplex virus (HSV), manifested by itchy rashes in the form of blisters (vesicles), which can occur on any part of the skin and mucous membranes. The infection rate of the world's population with HSV is extremely high, more than 95%.
There are two main groups of HSV: types 1 and 2 (HSV-1. HSV-11). HSV-1 most often causes lesions on the skin of the face (popularly called “fever” or “cold”) and upper extremities, while HSV-11 causes lesions on the genitals.
The journey of the virus in the body
The source of HSV infection is a patient or a virus carrier (there are no external manifestations of the disease, but the virus is excreted in saliva, urine, and discharge from the genitourinary system). The virus is transmitted by contact, airborne droplets, blood transfusions and organ transplants. During pregnancy, infection of the fetus can occur transplacentally (through the placenta) and during childbirth.
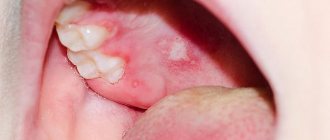
It has been established that in 40% of cases, primary HSV infection occurs by airborne droplets in early childhood, and the source of infection, as a rule, is family members who have active signs of herpes infection (usually recurrent herpes of the lips). The herpes simplex virus enters the body through injured skin or mucous membranes (red border of the lips, mucous membranes of the mouth, genitals, conjunctiva) - where typical blistering rashes appear (the result of the activity of the virus), and penetrates the bloodstream and lymphatic system. Viral particles reach the nerve nodes (ganglia) of the central nervous system, where they remain inactive for life. For example, with herpes of the face, the virus is stored in the ganglia of the trigeminal nerve, and with herpes of the genitals - in the ganglia of the lumbosacral spine. From the nerve ganglia, viral particles begin to move to the periphery - the skin, mucous membranes, and a focus of infection develops during a relapse.
Under certain conditions, HSV multiplies in lymphocytes (blood cells), which leads to their damage and disruption of the genetic mechanisms that control immune responses. Clinically, this manifests itself in frequent colds, decreased performance, weakness, increased body temperature, and enlarged lymph nodes.
A recurrent course of the disease is observed in 17-50% of the population infected with HSV. Exacerbations of herpes occur after various provoking factors: hypothermia, mental or physical trauma (dental, gynecological medical procedures), alcohol intake, against the background of hormonal surges (“menstrual herpes”). “Solar herpes” is known, which appears under the influence of ultraviolet rays.
However, it is worth noting that the herpes virus may never manifest itself as a disease during a person’s life.
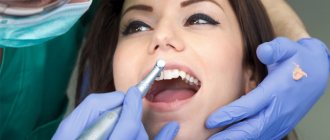
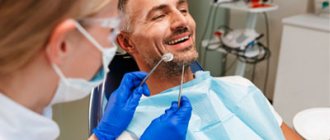
Possible consequences of dental treatment for herpes symptoms
The consequences of visiting the dentist during the period of herpes symptoms can be different.
Self-infection is the most common threat; infection can affect the oral cavity. As a result, the patient will have to fight inflammation much longer and experience discomfort. Infection can affect implants and prostheses, the replacement of which will have a significant impact on the family budget.
Additional infection is a consequence of injury to the inflamed areas. The dentist may accidentally damage the bubbles.
Any surgical intervention reduces immunity, tooth extraction is no exception; as a result, the body does not spend enough energy fighting herpes, and the recovery process is delayed. There is a high probability of additional lesions appearing.
The likelihood of negative consequences after visiting the dentist’s office is high, and in certain cases treatment cannot be postponed. Such cases include:
- acute toothache;
- rapid spread of infection in the oral cavity;
- purulent discharge on the gums;
- fever associated with teeth;
- tooth injury.
If it is not possible to reschedule a visit to the dentist, you should warn the specialist about the disease and provide information about the medications used. An experienced doctor will take measures to reduce the likelihood of complications after treatment.
The appearance of herpes after visiting the dentist is common. At the same time, you should not make spontaneous decisions or bring charges against a specialist. According to statistical studies, the manifestation of herpes after visiting the dentist in most cases is the result of stress. Fear and overexcitation negatively affect the state of the entire body and reduce protective functions. There is a possibility of infection with the virus in the dentist’s office; to avoid negative consequences, you should visit specialists with an impeccable reputation and focus on compliance with sanitary and hygienic standards.
Many-sided, insidious
The properties of HSV are such that almost all human organs can be involved in the infectious process, which allows us to speak of herpes as a “herpetic disease” with a predominant lesion of one or another organ system. For example, the eyes, ENT organs (pharynx, larynx, ear), lungs, genitals, gastrointestinal tract, central nervous system (meninges, nerves), skin and mucous membranes (face, lips, oral mucosa) may be affected. ) etc.
The frequency and intensity of exacerbations of recurrent herpes depend on the activity (aggressiveness) of the pathogen, as well as on the resistance of the human body.
Exacerbations of herpes infection are not always accompanied by the appearance of typical rashes in the form of blisters. The insidiousness of herpes lies in the fact that very often a person, without knowing it, becomes a source of infection for others. This applies to both facial herpes and genital herpes, which often manifests itself only in severe pain (in the facial area or in the pelvis, respectively).
When herpes worsens (when rashes appear), the patient becomes acutely contagious. Kissing a loved one or relative during an exacerbation can lead to the appearance of herpes in a previously healthy person. In addition, under unfavorable circumstances and failure to comply with personal hygiene rules, conditions for self-infection may arise. Thus, the virus can be carried from a lesion on the lips by hands into the eyes and genitals. In the presence of microtraumas in these areas, new foci of the disease arise: ocular herpes or genital herpes.
Genital herpes
Genital herpes (GG) is one of the most common infections of the genitourinary system, most often caused by HSV-11. Infection occurs through close physical contact with a patient or virus carrier during genital, oral-genital, genitorectal and oral-anal contact. There are primary and recurrent genital herpes.
With primary genital herpes, the incubation period (the period from infection to the appearance of the first symptoms of infection) is 1-10 days and differs from subsequent relapses in a more severe and prolonged course. Clinical symptoms of primary HH develop in only 10% of infected people and are characterized by the appearance on the mucous membranes of the genital organs and adjacent areas of the skin of single erosions or grouped small blisters filled with liquid, with redness around them. After 2-4 days, the contents of the blisters become cloudy, and they burst, forming weeping ulcers, which then heal. Subjectively, patients are bothered by itching, burning, and pain in the affected area. Some patients experience an increase in body temperature up to 38°C and a painful enlargement of the inguinal lymph nodes. If the course of the disease is favorable, after 5-7 days the crusts disappear and a stain remains in their place. Even without treatment, symptoms usually go away on their own within 2-3 weeks. Subsequently, for many, the disease recurs, and the time until the next relapse can range from several weeks to several years.
Recurrent genital herpes is characterized by a chronic course, disruption of the patient’s sexual and reproductive functions. The disease is difficult to treat. Herpetic rashes can appear on the labia majora and minora, vaginal mucosa, cervix, and perineum. The duration of the rash does not exceed 3-5 days. In some cases, during a relapse, visible rashes are not detected at all, but swelling, itching, and a feeling of discomfort in the genital area appear. The disease may be accompanied by fever, general weakness and malaise, enlargement and tenderness of the inguinal lymph nodes (usually on one side).
A feature of genital herpes is multifocality: the pathological process often involves the lower part of the urethra (urethra, bladder, which is manifested by pain and pain at the beginning of urination, frequent urination) and the mucous membrane of the rectum (recurrent cracks occur), as well as the upper parts of the genital tract (uterus, ovaries and fallopian tubes). In the latter case, the appearance of mucous discharge from the vagina, periodic pain in the pelvis, in the area of the projection of the uterus, ovaries (symptoms of irritation of the pelvic nerve plexus) are possible. Moreover, these symptoms are often associated with a certain phase of the menstrual cycle (with ovulation or the perimenstrual period). It is not uncommon that the viral nature of the disease is not recognized, and patients are treated for a long time by gynecologists with antibacterial and antifungal drugs to no avail.
When you need to treat your teeth even if you have a “cold” on your lip
Let's now look at situations where treating teeth in the presence of herpes on the lips is not only possible, but also necessary:
- urgent tooth extraction for herpes on the lip: that is, it is an urgent treatment (and not a planned one) - because the removal in this case alleviates the patient’s condition. And if the tooth is not removed, complications may begin, including hospitalization in the department of maxillofacial surgery and surgery,
- severe toothache that does not go away after taking painkillers,
- gumboil (periostitis) and gum decay,
- severe tooth decay, which is accompanied by various symptoms - pain, bleeding, headache, gum inflammation: this situation is possible when a natural crown is chipped or a prosthesis is displaced,
- high fever due to toothache or jaw pain.
Here, urgent removal is most often carried out, less often - installation of a temporary filling, opening of the periosteum to drain out purulent masses, removal of the damaged prosthesis (and its disinfection). Additionally, the dentist uses increased measures to maintain the sterility of the work area, and then sanitary cleaning and air quartzing are carried out in the room. The patient is prescribed medications to speed up rehabilitation - antibiotics, oral baths with a decoction of chamomile or oak bark.
“The child had a severe toothache at night; he couldn’t sleep at all. But analgin did not help. In the morning I called the dentist to figure out what to do. After all, the little one has a cold, and it’s contagious. But the hospital told me to bring him in and they’ll take a look. As a result, they pulled this tooth and there was pulpitis. And they prescribed a bunch more pills.”
Anna L., Ekaterinburg, review from otzonik.com
Complications of genital herpes
Complications of genital herpes include dryness and the formation of painful bleeding cracks on the mucous membranes of the external genitalia, which occurs due to mechanical stress (for example, during sexual intercourse).
A special place among other complications is occupied by pain syndrome caused by specific herpetic neuralgia of the pelvic nerve plexus. In this case, women complain of periodically occurring nagging pain in the lower abdomen, in the area of the projection of the ovaries, radiating to the lumbar region and rectum, pain in the perineum. Pain with recurrent herpes can occur regardless of the presence of skin rashes, which greatly complicates diagnosis. Recurrent genital herpes, disrupting the normal sex life of patients, often causes neuropsychiatric disorders and leads to conflicts in the family.
Genital herpes in some women causes miscarriage and infertility.
Diagnostics
If you suspect the presence of herpes simplex, you should not self-medicate. It is urgent, without delay or masking the rash, to come to an appointment with a dermatovenerologist. A carefully collected anamnesis (questioning of the patient) is important for establishing the correct diagnosis. Herpes, regardless of the location of the pathological process, is characterized by a wave-like course, when painful states are replaced by periods of well-being, even without treatment. The presence of blistering rashes on the skin and mucous membranes, severe subjective symptoms (itching, burning) allows doctors to visually diagnose herpes simplex, prescribe treatment in a timely manner and inform the patient about the danger of infecting a sexual partner.
Only laboratory research methods, which are fundamentally divided into two groups, can reliably confirm the herpetic nature of the disease in the absence of typical manifestations on the skin and mucous membranes:
- isolation and identification of HSV from infected material (material for analysis are scrapings from the lesion, blood, urine, saliva, tear fluid, cerebrospinal fluid, discharge of the cervical canal, vagina, urethra, rectum);
- detection of specific antibodies (protective proteins) to the herpes virus in blood serum - serodiagnosis.
Alarming symptoms after visiting the dentist:
- pain in the gums and lips, which gradually turns into a burning sensation;
- severe redness;
- the appearance of blisters on the lips.
If a patient encounters the problem of herpes for the first time, especially after visiting a dentist, it is impossible to do without qualified consultation. Self-medication can cause negative consequences; without practical experience it is difficult to make accurate diagnoses. Herpes is not the only viral disease that is accompanied by inflammatory processes and rashes on the lips. The duration and effectiveness of treatment depends on the accuracy of the diagnosis. Before and after visiting the dentist, you should carefully treat the inflamed areas on the lips and apply a special ointment.
Herpes is a common disease; an experienced dentist will approach the treatment competently, performing only manipulations that are impossible to do without. For example, acute toothache is a reason for immediate surgical intervention. Careful treatment prevents accidental injury to inflamed areas; the choice of a dental clinic should be taken responsibly; health depends on the level of qualifications of the doctor.
The dentist has the right to refuse treatment to patients with obvious manifestations of viral diseases in order to prevent the spread of infection and infection of other visitors to the clinic. You cannot insist on treatment and risk your own health and the safety of others. People whose main cause of herpes is nervousness are advised to start taking sedatives a few days before treatment.
Isolation and identification of HSV
In specialized virology laboratories, HSV is isolated using the culture method. Its essence lies in the fact that the material for research (the contents of herpetic eruptions, human secretions) is placed on specially grown cells in which the virus begins to multiply. Then, after 5 days, the presence of HSV is determined by characteristic changes. Thus, we can say for sure that this disease is of a herpetic nature.
To identify the causative agent of HSV, the polymerase chain reaction (PCR) method is widely used, which makes it possible to find out what type of herpes virus is present in the body. The material for research is taken with a special brush from the rash sites. The PNR method is highly sensitive and is performed within 24–48 hours.
Serodiagnosis
Antibodies to the herpes virus appear in the blood serum by 4-7 days after the initial infection, reach a peak after 2-3 weeks and can persist throughout life. The diagnosis is made by the characteristic increase in antibodies and determination of their class. For example, the detection of a certain level of immunoglobulin M (antibodies) indicates a primary infection of a person or an exacerbation of herpes. The detection of a certain level of immunoglobulin G indicates that the human body has encountered the virus and has developed antibodies - the person is infected, but not infectious to others. The result is known the next day. The analysis can be repeated at intervals of several days.
Herpes zoster and herpes-associated pain
Herpes zoster (HZ) is a sporadic disease that is the reactivation of a latent viral infection caused by the herpes virus type 3 (Varicella zoster virus (VZV)). The disease occurs with primary damage to the skin and nervous system.
VZV is the etiological agent of two clinical forms of the disease - primary infection (varicella) and its recurrence (herpes zoster). After a primary infection (chickenpox), usually in childhood or adolescence, the virus enters a latent state, localizing in the sensory ganglia of the spinal nerves. The commonality of the causative agent of chickenpox and herpes zoster was established even before the isolation of the virus using serological reactions in which liquid obtained from blisters on the skin of patients was used as an antigen. Later, using genomic hybridization, it was proven that in the acute period of herpes zoster, the detection rate of VZV is 70–80%, and in individuals without clinical manifestations, but with antibodies, viral DNA is detected in 5–30% of neurons and glial cells.
The prevalence of herpes zoster in different countries of the world ranges from 0.4 to 1.6 cases per 1000 patients/year in people under 20 years of age and from 4.5 to 11.8 cases per 1000 patients/year in older age groups. The lifetime risk of contracting herpes zoster is up to 20%. The main risk factor for its occurrence is a decrease in specific immunity to VZV, which occurs against the background of various immunosuppressive conditions.
Clinical picture of OH
The clinical picture of OH consists of skin manifestations and neurological disorders. Along with this, most patients experience general infectious symptoms: hyperthermia, enlarged regional lymph nodes, changes in the cerebrospinal fluid (in the form of lymphocytosis and monocytosis). Approximately 70–80% of patients with OH in the prodromal period complain of pain in the affected dermatome, which subsequently develops skin rashes. The prodromal period usually lasts 2–3 days, but often exceeds a week. Rashes with OH have a short erythematous phase, often completely absent, after which papules quickly appear. Within 1-2 days, these papules turn into vesicles, which continue to appear for 3-4 days - the vesicular form of herpes zoster. At this stage, elements of all types may be present on the skin. Elements tend to merge. Pustulation of vesicles begins a week or even earlier after the appearance of the first rash. After 3–5 days, erosions appear at the site of the vesicles and crusts form. If the period of appearance of new vesicles lasts more than one week, this indicates the possibility of an immunodeficiency state. The crusts usually disappear by the end of the 3rd or 4th week. However, peeling and hypo- or hyperpigmentation may remain for a long time after the resolution of OH.
Pain syndrome is the most painful manifestation of OH. While some patients experience rash and pain of relatively short duration, 10–20% of patients experience postherpetic neuralgia (PHN), which can last months or years, significantly reduces quality of life, causes great distress, can lead to loss of independence, and is associated with significant financial costs . Effective treatment of pain associated with OH is an important clinical goal.
Herpes-associated pain
According to modern concepts, pain syndrome in OH has three phases: acute, subacute and chronic. If in the acute phase the pain syndrome is mixed (inflammatory and neuropathic) in nature, then in the chronic phase it is typical neuropathic pain (Fig.). Each of the listed phases has its own treatment features, based on the pathogenetic mechanisms of pain and confirmed by controlled clinical studies.
Acute herpetic neuralgia
Pain in acute herpetic neuralgia usually occurs in the prodromal phase and lasts for 30 days - this is the time required for the rash to resolve. In most patients, the appearance of a rash is preceded by a burning sensation or itching in a specific dermatome, as well as pain, which can be stabbing, pulsating, shooting, paroxysmal or constant. In a number of patients, the pain syndrome is accompanied by general systemic inflammatory manifestations: fever, malaise, myalgia, headache. Determining the cause of pain at this stage is extremely difficult. Depending on its location, differential diagnosis should be made with angina pectoris, intercostal neuralgia, acute attack of cholecystitis, pancreatitis, appendicitis, pleurisy, intestinal colic, etc. The cause of the pain syndrome becomes obvious after the appearance of characteristic rashes. In typical cases, the prodromal period lasts 2–4 days, no more than a week. The interval between the onset of the prodrome and the onset of rash is the time required for reactivated VZV to replicate in the ganglion and be transported along the cutaneous nerve to nerve terminals at the dermoepidermal junction. The replication of the virus in the skin takes some more time, followed by the formation of inflammatory reactions. The immediate cause of prodromal pain is subclinical reactivation and replication of VZV in neural tissue. Experimental studies on animals have shown that at sites of VZV replication, the concentration of neuropeptide Y in nervous tissue, which is a marker of neuropathic pain, increases [1]. The presence of severe pain in the prodromal period increases the risk of more severe acute herpetic neuralgia and the likelihood of subsequently developing postherpetic neuralgia.
In most immunocompetent patients (60–90%), severe, acute pain accompanies the appearance of a skin rash. The severity of acute pain syndrome increases with age. Severe pain is also observed more often in women and in the presence of a prodrome. A characteristic feature of acute herpetic neuralgia is allodynia - pain caused by a non-painful stimulus, such as the touch of clothing. It is allodynia in the acute period that is a predictor of the occurrence of postherpetic neuralgia [2, 3]. The absence of allodynia, on the contrary, is a good prognostic sign and may suggest recovery within three months.
Subacute herpetic neuralgia
The subacute phase of herpetic neuralgia begins after the end of the acute phase and lasts until the onset of postherpetic neuralgia. In other words, this is pain that lasts more than 30 days from the beginning of the prodrome and ends no later than 120 days (Fig.). Subacute herpetic neuralgia can develop into postherpetic neuralgia. Factors predisposing to the continuation of pain include: older age, female gender, the presence of a prodrome, massive skin rashes, localization of rashes in the area of innervation of the trigeminal nerve (especially the eye area) or brachial plexus, severe acute pain, the presence of immunodeficiency [3, 4 ].
Postherpetic neuralgia
The International Herpes Treatment Forum defines PHN as pain lasting more than four months (120 days) after the onset of the prodrome. PHN, especially in older patients, can last for many months or years after the rash has healed. With PHN, three types of pain can be distinguished: 1) constant, deep, dull, pressing or burning pain; 2) spontaneous, periodic, stabbing, shooting, similar to an “electric shock”; 3) pain when dressing or lightly touching in 90%.
Pain syndrome is usually accompanied by sleep disturbances, loss of appetite and weight loss, chronic fatigue, and depression, which leads to social isolation of patients.
PHN is considered to be a typical neuropathic pain resulting from damage or dysfunction of the somatosensory system. Several mechanisms are involved in its pathogenesis.
- Nerve damage disrupts the transmission of pain signals, which leads to increased activity of higher order neurons (deafferentation hyperalgesia) [6–8].
- Nerve fibers damaged by VZV may generate spontaneous activity at the site of injury or other sites along the nerve (spontaneous ectopic activity of injured axons).
- Damage or inflammation of the nerve as a result of virus reactivation leads to a decrease in the threshold for activation of nociceptors, activation of urinary nociceptors—peripheral sensitization [5, 9].
- As a result of these changes in the peripheral parts of the somatosensory system, the activity of central nociceptive neurons increases and new connections are formed between them, provided that the pain continues—central sensitization [10–12]. The systems for recognizing pain and temperature stimuli are characterized by increased sensitivity to minor mechanical stimuli, causing severe pain (allodynia).
In most patients, pain associated with PHN improves within the first year. However, in some patients it can persist for years and even throughout the rest of their lives, causing considerable suffering. PHN has a significant negative impact on the quality of life and functional status of patients, who may develop anxiety and depression.
How to reduce the risk of PHN?
This issue is the most important for any doctor treating a patient with OH, and includes early initiation of etiotropic (antiviral) therapy and adequate pain relief in the acute stage.
Antiviral therapy. The results of many clinical studies have shown that the administration of antiviral drugs reduces the period of viral shedding and the formation of new lesions, accelerates the resolution of the rash and reduces the severity and duration of acute pain in patients with OH. Thus, in controlled studies using recommended dosages, the time to complete cessation of pain when prescribing famciclovir was 63 days, and when prescribing placebo - 119 days. Another study showed greater effectiveness of valacyclovir compared to acyclovir: pain syndrome when prescribed valacyclovir (Valavir) disappeared completely after 38 days, and when prescribed acyclovir after 51 days. Valacyclovir and famciclovir have similar effects on herpes-associated pain in immunocompetent patients [13, 23]. Thus, antiviral therapy is indicated not only for the rapid relief of skin manifestations, but also for the acute phase of the pain syndrome.
In all controlled clinical trials of antiviral therapy (
) it is recommended to start therapy within 72 hours of the onset of rash [1, 14].
The effectiveness of the anti-pain effect of antiviral therapy started at a later date has not been systematically studied, however, numerous clinical data suggest that late-started therapy can also affect the duration and severity of acute pain.
Antipain therapy. Effective relief of acute pain syndrome in OH is the most important stage in the prevention of PHN. It is advisable to stage-by-stage treatment of zoster-associated pain syndrome in all its phases. Thus, in the treatment of acute and subacute herpetic neuralgia, pain therapy consists of three main stages:
- Stage 1: Aspirin, paracetamol, non-steroidal anti-inflammatory drugs (NSAIDs);
- Stage 2: opioid analgesics, including tramadol;
- Stage 3: drugs with a central analgesic effect (tricyclic antidepressants, anticonvulsants).
Considering that in our country there are known organizational difficulties in prescribing opioid analgesics, if simple analgesics and NSAIDs are insufficiently effective, it is necessary to move on to prescribing drugs with central action.
Treatment of postherpetic neuralgia
Currently, there are 5 main groups of medications: anticonvulsants, tricyclic antidepressants, lidocaine patch, capsaicin, opioid analgesics [21].
Anticonvulsants: Gabapentin and pregabalin are the two most commonly used anticonvulsants for the management of neuropathic pain associated with PHN. Drugs are more often used at the beginning of the development of PHN to reduce the acute component of neuropathic pain. In one study [15], in patients taking gabapentin, 43.2% had a decrease in pain perception, compared with 12.1% in the placebo group. In a similar trial [16], pregabalin also reduced the number of patients with PHN, especially in those aged 65 years and older. Gabapentin and pregabalin appear to be equally effective in reducing neuropathic pain [17]. Gabapentin is the drug of first choice for the treatment of any type of neuropathic pain; it is one of the most well-studied and widely used drugs in neurologist practice for the relief of pain in PHN. It is a structural analogue of gamma-aminobutyric acid (GABA). Gabapentin enhances the synthesis of GABA by stimulating the activity of glutamate decarboxylase; modulates the activity of NMDA receptors; blocks a-2-d-subunits of voltage-dependent calcium channels and inhibits the entry of Ca2+ into neurons; reduces monoamine release and sodium channel activity; reduces the synthesis and transport of the excitatory neurotransmitter glutamate; helps reduce the frequency of action potentials in peripheral nerves. The concentration of gabapentin in the blood plasma reaches its peak 2–3 hours after administration, the half-life is 5–7 hours. The dosing interval should not exceed 12 hours, bioavailability is 60%. Eating does not affect the pharmacokinetics of the drug; antacids reduce its concentration in the blood, so gabapentin should be taken no earlier than 2 hours after taking antacids. Excreted in breast milk; The effect of the drug on the child’s body has not been studied. Adverse reactions develop extremely rarely: slight dizziness, drowsiness. Gabapentin enhances the effect of lidocaine and antidepressants. You should refrain from combining it with alcohol, tranquilizers, antihistamines, barbiturates, sleeping pills, and drugs. The drug has important advantages in the treatment of neuropathic pain: safety, low potential for interaction with other drugs, good tolerability, and is not metabolized in the liver. Gabapentin is the drug of choice for the treatment of elderly people during polypharmacotherapy; it is convenient to use and has been proven to be highly effective.
Gabapentin dosage regimen. Initial dose: 1st day 300 mg in the evening; 2nd day 300 mg 2 times (day and evening); Day 3: 300 mg 3 times. Titration: days 4–6 300/300/600 mg; 7–10 days 300/600/600 mg; Days 11–14 600/600/600 mg. Daily therapeutic dose 1800–3600 mg, maintenance dose 600–1200 mg/day.
Pregabalin has a mechanism of action similar to gabapentin, but does not require slow titration and is therefore more convenient for clinical use. The drug is prescribed twice a day. The initial dose is 75 mg twice, the daily therapeutic dose is 300–600 mg. Several randomized clinical studies of the effectiveness of pregabalin in postherpetic neuralgia have been conducted, which showed the rapid development of an analgesic effect (during the first week of administration), good tolerability, ease of use and a reduction in sleep disturbances associated with pain [22].
Antidepressants. Drugs in this group, especially tricyclics (nortriptyline and amitriptyline), are important components in the treatment of pain in PHN. Due to the activation of descending serotonin and norepinephrine antinociceptive systems and the ability to block sodium channels, antidepressants block the perception of pain. In clinical trials of the effectiveness of tricyclic antidepressants in reducing pain in PHN, 47% to 67% of patients reported “moderate to excellent” pain relief, with equivalent effects reported for amitriptyline and nortriptyline [17]. However, nortriptyline does not cause many anticholinergic effects and may therefore be preferable to amitriptyline.
A patch with 5% lidocaine is applied to the affected area at the beginning of chronic pain or immediately after the diagnosis of PHN is made. The patch is applied to intact, dry, non-inflamed skin. It is not used on inflamed or damaged skin (i.e. during active herpetic eruptions). Lidocaine is an antagonist of sodium ion channels, the analgesic effect develops as a result of preventing the generation and conduction of neuronal activity potentials, by binding sodium channels of overactive and damaged nociceptors. A patch with 5% lidocaine has a local effect and has almost no systemic effects. Several studies have shown that the lidocaine patch reduces pain compared with placebo [18]. Comparative studies of the effectiveness of 5% lidocaine and pregabalin showed their equal effectiveness [19]. Capsaicin, which is made from red peppers and is an irritant, is used as an ointment or patch. When applied to the skin, it depletes peptidergic neurotransmitters (eg, substance P) in primary nociceptive afferents. The drug should be applied to the affected area 3-5 times a day to maintain a long-term effect. Despite the fact that a number of studies have shown the effectiveness of capsaicin against PHN, many patients often experienced significant adverse reactions: for example, a third of patients reported the development of an “unbearable” irritant effect of the drug, which significantly limits its clinical use in PHN.
Opioid analgesics (oxycodone, methadone, morphine) can also be used in the treatment of PHN. They reduce neuropathic pain by binding to opioid receptors in the central nervous system or inhibiting the reuptake of serotonin or norepinephrine at peripheral nerve endings - nerve synapses. According to research results, oxycodone, compared with placebo, provides greater pain relief and reduces the severity of allodynia, but causes the development of adverse reactions such as nausea, constipation, drowsiness, loss of appetite, and drug dependence [20]. Comparative studies of the effectiveness of opioids and tricyclic antidepressants have demonstrated their equivalent effectiveness.
In the section “Treatment of postherpetic neuralgia” in the 2009 European guidelines [21] for the treatment of neuropathic pain, first-line therapy is distinguished (drugs with proven effectiveness - class A): pregabalin, gabapentin, lidocaine 5%. Second-line drugs (class B): opioids, capsaicin.
When treating patients with PHN, it is advisable to follow certain steps.
Initially, first-line drugs are prescribed: gabapentin (pregabalin), or TCAs, or local anesthetics (plates with 5% lidocaine). If it is possible to achieve good pain reduction (VAS pain score – 3/10) with acceptable side effects, then treatment is continued. If pain relief is not sufficient, another first-line drug is added. If first-line drugs are ineffective, second-line drugs can be prescribed: tramadol or opioids, capsaicin, non-pharmacological therapy. In the complex therapy of postherpetic neuralgia, non-pharmacological therapy is also used: acupuncture, TENS anesthetic device, the most promising and effective method is neurostimulation.
Treatment of PHN is extremely challenging. Even with the use of various pain medications and referral to a specialist algologist, it is not always possible to achieve the disappearance of the pain syndrome.
Literature
- Dworkin RH Johnson RW, Breuer J., Gnann JW, Levin MJ Recommendation for management of herpes zostritis // Cln Infec Dis. 2007; 44: (Supl 1): S1–S26.
- Dworkin RH, Nagasako EV, Johson RW, Griffin DR Acute pain in herpes zoster: tue famciclovir database project // Pain. 2001; 94: 113–119.
- Hope-Simpson RE Postherpetic neuralgia // JR Coll Gen. Pract. 1975; 157:571–675.
- Choo P., Galil K., Donahue JG Walker et al. Risk factors for postherpetic neuralgia // Arch. Intern. Med. 1997; 157:1217–1224.
- Garry EM, Delaney A, Anderson HA et al. Varicella oster virus induces neuropathic changes in rat dorsal root ganglia and behavior reflex sensitization that is attenuated by gabapentin or sodium channel blocking drugs // Pain. 2005; 118:97–111.
- Yung BF, Johnson RW, Griffin DR, Dworkin RH Risk factors for postherpetic neuralgia in patients with herpes zoster // Neurology. 2004; 62:1545–1551.
- Jonson RW Zoster-associated pain: what is know, who is at risk and how can it be managed? // Herpes. 2001, 14 Supplement; 2:31A–34A.
- Tal. M., Bennett GJ Extra territoiral pain in rats with a peripheral mononeuropathy: mechano-hyperalgesia and mechano-allodenia in the territory of an uninjured nerve // Pain. 1994; 57:375–382.
- Oaklander AL The density of remaining nerve endings in human skin with and without postherpetic neuralgia after shingles // Pain. 2001; 92: 139–145.
- Rowbotham MC, Yosipovitch G., Connoly MK, Finlay D., Forde G., Fields HL Cutaneus innervation density in allodynic from postherpetic neuralgia // Neurobiol. Dis. 1996; 3:205–214.
- Rowbotham MC, Fields HL The relationship of pan, allodynia and thermal sensation in post-herpetic neuralgia // Brain. 1996; 119(Pt2):347–354.
- Scholz J., Broom DC, Youn DH, Mills CD, Kohno T. et al. Blocking caspase activity prevents transsynaptic neuronal apoptosis and the loss of inhibition in lamina 11 of dorsal horn afer peripheral nerve injury // J Neurosci. 205; 25:7317–7323.
- Tyring SK, Beutner KR, Tucker BA et al. Antiviral therapy for herpes zoster. Randomized, controlled clinical trial of vlacyclovir, and farmavir therapy in immunocompetent patients of 50 years and older // Arch Farm Med. 2000; 9:863–869.
- Gross G., Schofer H. et al. Herpes zoster guideline of German Dermatology Society (DDG) // J of Clinical Virology. 2003; 26:277–289.
- Rowbotham M., Harden N., Stacey B. et al. Gabapentin for the treatment of postherpetic neuralgia: a randomized controlled trial // JAMA. 1998. Vol. 280. P. 1837–1842.
- Dworkin R., Young J., Sharma U. et al. Pregabalin for the treatment of postherpetic neuralgia: a randomized, placebocontrolled trial // Neurology. 2003. Vol. 60. P. 1274–1283.
- Stankus S., Dlugopolski M., Packer D. Management of herpes zoster (shingles) and postherpetic neuralgia // Am Fam Physician. 2000. Vol. 61. P. 2437–2444.
- Karly P. Garnock-Jones, Gillin M. Keating/Lidocain 5% Medical Plaster. A review of its use in hjsterpetic neuralgia // Drugs. 2009; 69(15):2149–2165.
- Rehm S., Binder A., Baron R. Post-herpetic neuralgia: 5% lidocain medicated plaster? Pregadflin, or a combination both? A randomized, open/clinical effectiveness study // Cur. Med. Reas. 2010, v. 26, no. 7.
- Watson C., Babul N. Efficacy of oxycodone in neuropathic pain: a randomized trial in postherpetic neuralgia // Neurology. 1998. Vol. 50. P. 1837–1841.
- Attal N. et al. EFNS guidelines of the pharmacological treatment of neuropathic pain: 2009 revision // European Journal of Neurology. 2010.
- Seventer R., Feister H. et al. Efficacy and tolerance of twice-daily pregabalin for treating pain and related sleep interference in postherpetic neuralgia: a 13-week, randomized trial // Curr Med Res Opin. 2006; 22 (2): 375–384.
- Beutner KR et al. Valaciclovir compared with acyclovir from improved therapy for herpes zoster in immunocompetent adults // Antimicrobal agents and chemotherapy. 1995, July, vol. 37, no. 7, p. 1546–1553.
E. G. Filatova, Doctor of Medical Sciences, Professor First Moscow State Medical University named after. I. M. Sechenova, Moscow
Contact information about the author for correspondence
Table.
Principles of treatment
Herpes can and should be treated. Currently, medicine has a whole arsenal of drugs that, in most cases, make it possible to obtain a lasting clinical effect in those who suffer from recurrent herpes and to successfully control periods of activation of the disease in asymptomatic forms. It is impossible to achieve complete removal of the virus from the body using currently existing treatment methods; it is possible to maintain the body in a state where the virus does not have a chance to activate. Currently, there are two main directions of treatment for herpes simplex:
- The use of antiviral drugs, the main place among which is occupied by acyclovir-containing (ACV) drugs. In case of exacerbation of herpes, the first aid remedy is medications containing acyclovir: ZOVIRAX, VAPTREX, ACICLOVIR-ACRI, VIROLEX. They are available in the form of tablets and creams. The same drugs are used locally in the form of cream and ointment. Taking these medications should begin in the first hours of an exacerbation.
- A complex treatment method that includes immunotherapy in combination with antiviral therapy. As a rule, the disease occurs against the background of suppressed immune reactions, so immunotherapy plays an important role in the treatment of herpes. If relapses of the disease are seasonal (autumn, spring) and they are accompanied by symptoms of ARVI, then to antiviral treatment with drugs containing acyclovir, it is advisable to add a course of drugs that stimulate the synthesis of interferon (a substance produced by the body and providing an antiviral effect): herbal immunostimulants (for example, IMMUNAL) and synthetic drugs such as ARBIDOL, AMEXIN, VIFERON, KIPFERON. Moreover, they can be used for preventive purposes about a month before the onset of autumn slush and spring hypovitaminosis). If relapses of herpes (at any location) occur more than 3-4 times a YEAR, this is a reason to consult a doctor. This means that the body's defenses (immunity) cannot cope with the infection. In such cases, after studying the immune status, the patient is prescribed complex treatment, including antiviral and immune drugs. In patients with recurrent herpes, the drugs TACTIVIN, TIMALIN, THIMOGEN, MYELOPID, etc. are successfully used (treatment must be carried out after an immunological study).
Should you visit the dentist if you have herpes?
A laconic description of the characteristics of herpes will help you form an idea of the possible consequences of treatment at the dentist. A qualified doctor will refuse to provide services to a patient and will begin treatment in exceptional cases. Herpes is a common chronic disease, the frequency of manifestation depends on lifestyle, characteristics of the body, and heredity.
Reasons for exacerbation:
- weakened immune system;
- colds, consequences of a viral disease;
- emotional exhaustion, tendency to depression;
- menstruation;
- abuse of strong drinks, smoking;
- poor nutrition, lack of vitamins;
- pregnancy;
- intoxication of the body;
- physical and emotional overload.
It is impossible to completely overcome the disease. The correct choice of treatment method will reduce the duration of inflammatory processes and reduce the frequency. It is practiced to use drugs for internal and external use; it is recommended to undergo an examination and consult a qualified specialist. If possible, you should discuss the possibility of visiting a dentist with a doctor who has selected a method for treating herpes.
It is impossible to remove a herpes infection from the body; everyone, even a healthy person, has the virus. In a dormant state, herpes is safe, does not cause inconvenience, and can appear often or only after serious illnesses. Herpes can appear the day before visiting the dentist; a peculiar protective function of the body, fear of upcoming procedures stimulates inflammatory processes. If herpes appears within a few days, ideally you should reschedule your visit to the dentist. For a quick recovery, it is recommended to discuss the causes of exacerbation of the disease with a doctor and select effective means that stimulate recovery processes.