2020 Michael Solomonov DMD, Alex Lvovsky DMD, Vered Katzenell DMD, Joe Ben Itzhak DMD, Elena Lipatova, Yehuda Zadik DMD, MHA
(.pdf)
Drug-induced osteonecrosis of the jaw (MRONJ)1 is an emerging area in endodontic practice. The article briefly reviews the currently available literature on the topic, compiles the current list of treatments that lead to MRONJ, and offers practicing endodontists a framework for identifying patient predisposition factors for MRONJ.
Osteonecrosis of the jaw
The MRONJ is defined by the American Association of Oral and Maxillofacial Surgeons (AAOMFS) [9] and the American Society for Bone and Mineral Research [10] as the area of exposed bone ( or exposed bone, or bone that can be probed through an intraoral or extraoral fistula [9] in the maxillofacial area that does not heal within 8 weeks of discovery by a healthcare professional [10], in a patient who has received or has been exposed to anti- resorptive (or anti-angiogenic [9]) medications and who have not received radiation therapy to the craniofacial area (or obvious metastatic disease to the jaw [9]).These organizations have developed stepwise systems for MRONJ with suggested treatments at each step:
- Stage 0: There is no exposed bone and no dead areas are found on the x-ray. Prescribe treatment depending on symptoms and control of local factors;
- Stage 1: Exposed bone or fistula leading to bone, but no signs of infection. Should be treated by rinsing the mouth with antiseptic solutions (eg chlorhexidine digluconate), surgical intervention is not indicated;
- Stage 2: exposed bone or fistula leading to bone, with signs of infection (usually symptoms). Therapy with antimicrobial mouth rinses and systemic antibiotics (eg penicillin) is necessary;
- Stage 3: exposed bone with complications such as pathological fractures, oroantral communication, or additional oral fistulas. They can be treated with surgery, including resection in combination with antibiotics [9, 10]. (Fig. 1).
Symptoms
The difficulty of diagnosing necrosis in the early stages of development is due to its similarity with other types of diseases. In addition, in the initial phase, the pathology can be asymptomatic, exacerbating only after the general state of immunity has weakened, or with the beginning of the process of destruction of the bone structure.
Characteristic signs of necrosis include:
- Painful sensations in the affected tooth;
- Increased pain with pressure;
- Excessive mobility of adjacent units;
- Swelling of mucous tissues;
- Isolation of purulent formations from gum pockets;
- Bad breath;
- Increased size of lymph nodes;
- Problems opening the jaw;
- Pain when swallowing and respiratory dysfunction;
- Loss of sensitivity of facial tissues;
- Violation of facial symmetry.
If there is systematic pain in the tooth, radiating to the fundus of the eye, back of the head or ear, detection of purulent discharge, as well as a feeling of excessive mobility of the element, it is recommended to immediately make an appointment for diagnostics at a dental clinic.
Diagnosis methods
The list of methods used includes standard procedures, such as radiographic examination, blood analysis and bacteriological culture, which determines the structure of the contents of the area of suppuration. According to the accepted classification, necrosis is divided into traumatic, hematogenous and odontogenic forms. In addition, as part of the diagnosis, the degree of damage is determined - four degrees are distinguished, from 10% to more than 70%.
Methods of therapy
The complexity of the pathology determines the duration of treatment. However, in cases where contacting a doctor was timely, the prognosis for the outcome of the therapeutic course is usually considered positive.
First of all, the dentist, based on the clinical picture, removes the original source of suppuration. Tooth extraction opens access to pathogenic formations, which are treated with an antiseptic and agents that stimulate tissue regeneration. To strengthen weakened adjacent units, it is possible to install a splint that fixes the teeth until complete restoration.
List of medications that can cause osteonecrosis of the jaw
A list of drugs that can cause MRONJ has been compiled, evidence and reports have been collected, and an increasing number of non-bisphosphonate drugs are now known to be associated with it, either by themselves or by increasing the risk associated with bisphosphonate MRONJ; Thus, some medications do not cause MRONJ unless they are given with a bisphosphonate, and the patient is then at higher risk of developing osteonecrosis of the jaw compared to patients taking a bisphosphonate alone.
In addition to bisphosphonates, the list of such medications includes denosumab, bevacizumab, sunitinib.
Cases of MRONJ have also been associated with the following medications: aflibercept, azacitidine everolimus, imatinib, pazopanib, sorafenib, tocilizumab and trastuzumab and have been described (Table 1) [9, 11–19]. Consequently, the AAOMFS changed the term for this phenomenon from bisphosphonate-dependent to drug-dependent MRONJ [9]. Table 1. List of medications that can cause the development of MRONJ
| Category | A drug | Commercial name | Main indicators | Mechanism of action | Risk level |
| Antiresorptive | Pamidronate | Aredia | Bone malignancies | Bisphosphonate (IV) | High |
| Zolendronate | Zometa, Aclasta | Bone diseases and malignancies | Bisphosphonate (IV) | High | |
| Alendronate | Fosalan, Fosamax | Bone diseases | Bisphosphonate (oral) | Moderate | |
| Ibandronate | Boniva | Bone diseases | Bisphosphonate (oral) | Moderate | |
| Risedronate | Actonel, Atelvia, Benet | Bone diseases | Bisphosphonate (oral) | Moderate | |
| Denosumab | Prolia, Xgeva | Bone diseases and malignancies | RANKL inhibitor | High | |
| Targeted therapy | Bevacizumab | Avastin | Malignant formations | VEGF inhibitor | High |
| Sunitinib | Sutent | Malignant formations | Tyrosine kinase inhibitor | High | |
| Imatinib | Gleevec | Malignant formations | Tyrosine kinase inhibitor | Unknown* | |
| Pazopanib | Votrient | Malignant formations | Tyrosine kinase inhibitor | Unknown* | |
| Sorafenib | Nexavar | Malignant formations | Kinase inhibitor | Unknown* | |
| Tocilizumab | Actemra, RoActemra | Autoimmune diseases | Interleukin-6 receptor antibody | Unknown* | |
| Trastuzumab | Herceptin | Malignant formations | HER2/neu receptor antibody | Unknown* | |
| Azacitidine | Vidaza | Myelodysplasia | Nucleotide Analog | Unknown* | |
| Everolimus | Zortress, Certican, Afinitor, Votubia, Evertor | Malignancies and prevention of organ rejection | mTOR inhibitor | Unknown* | |
| Aflibercept | Eylea, Zaltrap | Colorectal malignancies | VEGF inhibitor | Unknown* |
*Only in documented cases.
Identification of patients at risk
Identification of a dental patient at risk is achieved through a thorough review of the medical history, the use of a structured questionnaire, an interview with the patient, and close interaction with the patient's previous treating physicians regarding the presence of current diseases and medication use on an ongoing basis [20]. Although, since bisphosphonates may not be prescribed on a daily basis (for example, weekly, bimonthly or monthly, or intravenously once a year), the patient and even his or her primary care physician may not consider these medications to be “continuous medications” [21]. , 22]. Moreover, those patients who no longer take bisphosphonates are still at risk of developing osteonecrosis of the jaw [9], but they will not list this drug in the medication column unless the dentist asks the patient about the medications that were taken previously [22]. Consequently, the fact that these drugs are being taken may be overlooked and a patient at risk may not be identified. Situations have been identified where a patient does not remember the names of previously taken medications, especially if there were several of them, as well as cancer patients who have been prescribed many medical protocols over the past years. The dentist should be familiar with the indications for the use of these medications and seek information from reliable sources about previous medication use (for example, hospital records), especially with patients who suffer from the following diseases: multiple myeloma associated with metastatic or osteolytic lesions, malignant tumors (such as breast, prostate or lung cancer), cancer-related hypercalcemia, osteoporosis, osteopenia, chronic corticosteroid administration, Paget's disease, osteogenesis imperfecta, juvenile osteoporosis, fibrous dysplasia and Gaucher disease [23].
Another possible reason for failure to identify an at-risk patient is non-bisphosphonate medications, which are associated with the development of MRONJ. Even those dentists who are familiar with the harmful effects of bisphosphonates may not be aware of these medications. Thus, dentists may miss these patients even if the person or their physician has provided a complete medical history [20]. Therefore, the dentist should be aware of the increased risk of osteonecrosis of the jaw associated with the above-mentioned drugs, as well as keep up to date with the latest research on this topic, since it is likely that new drugs will be added to this list of MRONJ-causing drugs in the future.
What are the causes of ONJ?
ONJ is a rare but serious side effect of certain medications that affect bone tissue. These include the medications denosumab and bisphosphonates. You may be prescribed these medications if you have:
- multiple myeloma or other types of cancer;
- cancer spreading to bone tissue;
- osteoporosis or osteopenia - diseases in which bone strength decreases, which can lead to bone fractures.
Medicines bisphosphonates
Bisphosphonates can be given orally (by mouth) or intravenously (through a vein). Here are some examples of bisphosphonates:
- Zoledronic acid (known as Zometa® for the treatment of cancer and Reclast® for the treatment of osteoporosis);
- Pamidronate disodium (Aredia®);
- Alendronate (Fosamax®);
- Risedronate sodium (Actonel®);
- Ibandronate sodium (Boniva®).
Medicines Denosumab
Denosumab is given by injection (shot). Examples of denosumab:
- Xgeva® for cancer treatment;
- Prolia® for the treatment of osteoporosis.
Both bisphosphonates and denosumab are used in higher doses and for longer periods in cancer patients than in those with osteoporosis.
to come back to the beginning
Treatment plan for an at-risk patient
In patients with a history of taking bisphosphonates or other mentioned medications, MRONJ may occur after oral surgical procedures, due to local inflammation, or without any objective cause [24–26]. There is also a risk of developing osteonecrosis of the jaw around long-standing osseointegrated dental implants, even if bisphosphonates were started long after successful osseointegration [27, 28].
Therefore, in accordance with the AAOMS protocol [9], when working with patients undergoing intravenous bisphosphonates (bevacizumab, denosumab or sunitinib), any surgical procedures, including tooth extraction, implant placement, apical surgery, etc., should be avoided. d. In patients who have been taking oral bisphosphonates for more than 4 or less than 4 years but who have other risk factors for developing MRONJ (eg, long-term corticosteroid therapy, chronic anemia, unbalanced diabetes mellitus, or other conditions that affect wound healing), the dentist should consider the need for dental surgery, including apical surgery, and if surgical manipulation is necessary, then the prescription of drugs should be considered with the attending physician [9], along with atraumatic procedures, a course of antibiotics and local antiseptic treatment. Some clinicians perform surgery only in at-risk patients whose serum c-terminal peptide levels are >150 μg/m2 [29, 30].
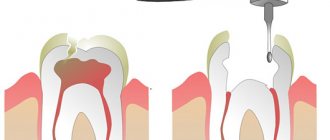
To avoid surgery in at-risk patients, clinicians should attempt to preserve their teeth even if they are considered unrestorable; The recommended manipulation of such teeth is root canal treatment (or retreatment, if necessary), closing the canal with a restorative material (for example, amalgam or glass ionomer cement) and performing decoronation (that is, filing the coronal part to the level of the gum) (Fig. 2).
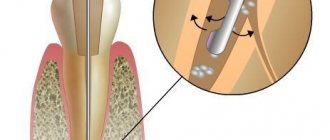
The fact that osteonecrosis of the jaw can appear around dental implants many years after successful osseointegration [27, 28] (Fig. 3) calls for a paradigm shift. The practice of removing teeth with various lesions and installing implants in their place without attempting to cure the tooth should be stopped. Premature removal and implantation in young patients may have consequences much later when that patient begins taking (orally or intravenously) a bisphosphonate or other MRONJ-promoting drugs for adult-onset disease.
How many people develop ONJ?
ONJ develops in only a small number of patients taking bisphosphonates or denosumab. We cannot predict who will have it and who will not.
Research suggests that ONJ develops in about 1 to 2 percent of patients (1 to 2 people in 100) who take these medications to treat bone cancer. The risk is much lower in patients taking these medications to treat osteoporosis. Research suggests that ONJ will occur in less than 1% of patients (about 1 in 10,000 to 1 in 100,000).
to come back to the beginning
MRONJ and endodontic manipulations
Apical periodontitis
As mentioned previously, MRONJ may occur after oral surgery or due to local inflammation (eg periodontitis) [25]. In particular, ONJ can manifest itself due to an inflammatory process in the alveolar bone, such as apical periodontitis (Fig. 4) [31]. Since endodontic treatment in itself does not increase the risk of developing MRONJ, while apical periodontitis does, endodontic treatment is indicated, especially before the prescription of antiresorptive drugs.
Apical surgery
Since all surgical procedures, to one degree or another, involve working with the bone tissue of the jaw, there is a risk of developing osteonecrosis after apical surgery in patients who took the previously mentioned drugs, as well as after apical periodontitis. It is also worth taking into account the indications for this surgical procedure. If surgery is indicated, the surgeon should adhere to the guidelines described above in the section on surgical planning.
Subgingival clasps
During endodontic treatment of a high-risk patient, the dentist should not use subgingival clasps for rubber dam isolation, since the use of this type of clasp can damage oral tissue and cause MRONJ [32]. Currently, there are multiple atraumatic techniques for isolating teeth, with or without clasps, such as ligature bonding, spit dam techniques, core restoration using a supragingival clasp, and the use of a projection technique for approaching canals [33–35].
Vertical root fracture
Vertical tooth root fracture requires special attention, since there is currently no effective therapy to save such teeth. Among endodontically treated teeth that were extracted, 10–36% were extracted due to vertical root fracture [36, 37]. Multiple manipulations during endodontic therapy and prosthetics can cause fracture, including factors such as excessive dentin removal [38], the destructive effect of chemicals [39, 40] and inappropriate obturation techniques [41, 42]. Factors associated with prosthetic restoration include additional dentin removal, the creation of permanent stress on the root dentin [43], and inappropriate selection of intracanal materials [44].
The occurrence of a vertical root fracture in a patient at risk for developing MRONJ is a mystery because removal of the affected tooth may result in osteonecrosis of the jaw [45], but preservation of the tooth may also lead to MRONJ due to inflammation of the surrounding bone tissue (in addition to deterioration of bone quality). life due to acute pain). Vertical fracture is the only indication for tooth extraction in at-risk patients, although clinicians should adhere to strict methodology, including atraumatic techniques (referral is also recommended), systemic local antimicrobial treatments, and avoidance of filling the socket with any intended materials.
As always, prevention is the best approach to preserving tooth vitality [46], but if this is not possible, then the use of a minimally invasive endodontic and prosthetic approach is mandatory [47]. Minimally invasive endodontic techniques include conservative access cavity preparation [48], avoidance of instruments with a taper greater than 6% [49–51], and avoidance of large apical extensions [52, 53]. Moreover, the emphasis should be on tools and techniques that reduce the risk of microcrack formation [54–56]. The use of medium concentration (i.e. 2.5–3.5%) sodium hypochlorite is recommended [39, 40]. If necessary, short-term investments of calcium hydroxide are possible according to indications [57], but for a period of no more than 1 month [58]. During the obturation process, the use of NiTi spreaders [59] and pre-fitted pluggers [60, 61] is recommended.
In prosthetic aspects, intracanal structures should be avoided [62, 63] or, if absolutely necessary, the space should be prepared by removing obstructive material with a heat plugger [64]. The channel for the anchor pin/cast inlay should be prepared to the maximum length [65] that will not compromise apical sealing [66, 67] and unnecessary removal of healthy dentin [64]. Bonding of a cast inlay is recommended with a venting (groove) to avoid stress in the root dentin [68].
Pathological picture
Computed tomography of a jaw affected by phosphorus necrosis.
The pathological process first affects the periosteum. Following its thickening, bone growths develop, osteophytes are observed, sclerosis of dying bone areas and detachment of periosteal integuments occur. The sequestra are washed by purulent compartments. Unlike osteomyelitis, however, demarcation of the process does not occur everywhere and not from all sides; the disease also invades neighboring healthy areas and, finally, necrotizes even the layer of newly formed periosteal growths. If the sequestral capsule manages to be freed from its contents in a timely manner, then the possibility of more or less perfect regeneration from the surviving periosteum cannot be excluded. In particularly favorable cases, reconstruction can even go as far as a relatively complete restoration of the articular processes of the lower jaw.
conclusions
The advent of MRONJ is changing modern dental practice. Despite relatively little attention in the endodontic literature, endodontics itself plays an important role in preventing the development of MRONJ through maintaining the integrity of the dentition, proper preparation of teeth before starting medications, and competent management of patients at risk. Endodontic treatment and decoronation of non-restorable teeth as an alternative to tooth extraction is a powerful tool in preventing the development of MRONJ in at-risk patients. The endodontist should identify such patients as early as possible, as well as MRONJ lesions.
As mentioned earlier, osteonecrosis of the jaw can develop many years after surgery, even if the procedure was performed while the patient was not
under the influence of antiresorptive treatment. This incredibly important discovery has enormous implications for dental practitioners, as teeth treated incorrectly in the past can lead to significant problems and suffering for the patient in the future. As patients get older every year, more and more of them may begin to require antiresorptive therapy. Great care must be taken to preserve the natural structure of the teeth by using minimally invasive dental procedures on all patients to reduce the susceptibility to vertical root fracture. Finally, the endodontist should consider MRONJ when diagnosing maxillofacial and oral pain in at-risk patients, even if there is no exposed oral bone.
Diagnostics
Symptoms of osteonecrosis of the jaw are similar to other diseases: tumors, bone tuberculosis, actinomycosis. Therefore, the examination is carried out comprehensively:
- History taking
If the patient has had osteomyelitis, is taking high doses of bisphosphonates, has undergone radiation therapy, or has had a jaw injury, the doctor will conduct additional examination. It will confirm or deny the presence of necrosis.
- Dental examination
If the bone is exposed, then the diagnosis is easier to make, but if the disease is at stage zero, additional data is needed.
- Lab tests
Positive tests for c-reactive protein, leukocytosis, high ESR are reasons to suspect a necrotic process. The urine is also checked for the presence of protein and blood cells. In some cases, purulent discharge is analyzed to identify the pathogen before prescribing bacterial therapy.
- X-ray
X-ray, or better yet, CT (computed tomography) helps determine the area of the pathological process, the degree of damage, the presence of fractures, sequesters (dead bone fragments lying freely between healthy tissues).