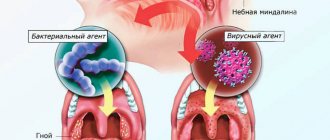
Herpangina is one of the most common viral diseases in children. Almost everyone experiences this disease in childhood, although this diagnosis also occurs in adults. From a scientific point of view, the very name “herpetic sore throat” was incorrectly given to the disease. Previously, the disease was little studied. Scientists, noticing the similarity of rashes during the disease with those of herpes, came to the conclusion that the causative agent of the disease was the herpes virus, and gave the disease a name that has stuck and is found in the medical literature in exactly this form. Although the disease has nothing in common with herpes infection. It has been established that the cause of herpetic sore throat is enteroviruses - Coxsackie viruses of groups A and B and ECHO viruses (echoviruses). In medical reference books you can find different versions of the names of this disease: aphthous tonsillitis, vesicular pharyngitis, herpetic tonsillitis, herpangina, etc.
As already mentioned, children under ten years of age are at risk: infants, preschoolers and children of primary school age. The severity of the disease depends on the age of the child. The disease is most severe in children in the first year of life. Preschoolers are more often infected because at this age they do not pay due attention to hygiene, have contact with animals and are often in children's groups. To become infected, it is enough to eat unwashed fruit. This should also include the immaturity of immunity at an early age. The disease is highly contagious, and often its outbreaks become epidemic. It is noteworthy that this disease does not occur in babies in the first months of life - the antibodies found in mother's milk create some kind of immunity to herpangina.
One can trace the obvious seasonality of herpetic sore throat: the peak occurs in summer and autumn. As a rule, having been ill once, a child becomes immune to re-infection, so this disease is less common among adolescents and adults.
Infection can occur in one of three ways:
- airborne
- contact
- fecal-oral.
With the airborne method, infection occurs by sneezing, coughing, or talking with a carrier of the virus. In case of contact - through discharge from the nasopharynx. With the fecal-oral method - through dirty hands, through unwashed food, toys and pacifiers, which is especially typical for children.
Even a recovering person can still spread the infection around him for about a month, so it is believed that herpes sore throat is highly contagious: a child can easily become infected in kindergarten from a baby who does not even have obvious symptoms of the disease. If one family member gets sick, most likely everyone will suffer from the disease.
How does infection spread throughout the body? First, the virus from the nasopharynx reaches the intestinal lymph nodes through the lymph flow. Already in the intestines, the virus gains strength and enters the blood, and severe inflammation begins in the oropharynx.
Symptoms of the disease
Herpes sore throat in a child does not manifest itself for seven to fourteen days. This is the incubation period for the disease. Then symptoms appear that are similar to those of other infectious diseases: acute respiratory infections, acute respiratory viral infections, influenza, intestinal infections - therefore, at the initial stage, herpetic sore throat is difficult to diagnose:
- high temperature up to 40°C
- severe sore throat, sore throat, cough
- Gastrointestinal disorders (vomiting, diarrhea, abdominal pain)
- muscle pain
- enlarged lymph nodes in the neck
- In infants, convulsions are possible.
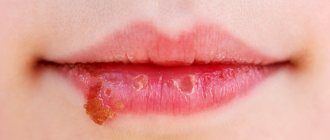
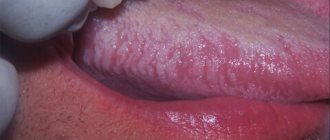
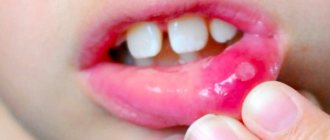
Abdominal pain and digestive disorders are associated with the activity of enteroviruses in the intestines that cause herpes sore throat - they affect the intestinal and stomach mucosa, thereby disrupting their functioning. On the second or third day of illness, a characteristic rash appears on the palate and tonsils, similar to blisters with liquid. The appearance of these rashes is a sign that we are dealing with herpetic sore throat. When these bubbles burst, they form ulcers, which create discomfort and pain in the mouth. A child experiencing severe sore throat may refuse not only food, but also drink. Increased salivation is possible, since the receptors that affect saliva production are constantly irritated.
If the baby has a weak immune system, the formation of bubbles can occur in several “passes” and with a break of two to three days, accompanied by a repeated increase in temperature and symptoms of intoxication. There are cases when rashes appear on the legs, arms and body, but not on the face.
The fever usually subsides on the third to fifth day, and mouth ulcers disappear within a week. When the peak of the disease passes, the child feels significant relief - improvement occurs on the sixth or seventh day after the appearance of the first symptoms. But we must remember that for a certain period the child remains a source of infection! One of the differences between herpes sore throat and acute respiratory infections is the absence of nasal discharge, although swelling of the mucous membrane is present. Also, outbreaks of acute respiratory infections and acute respiratory viral infections in the summer, as a rule, do not happen, which cannot be said about this type of sore throat. In summer, heat contributes to the rapid spread and high activity of enteroviruses, and the number of cases of herpangina increases accordingly.
Normally, herpetic sore throat in children lasts from eight to ten days.
Dear parents! Diagnosis and treatment of herpetic sore throat in children must be carried out under the supervision of an otorhinolaryngologist, since it is not always possible to make a correct diagnosis on your own (due to the similarity of the initial symptoms of the disease with other viral diseases). Failure to start proper treatment on time can result in a protracted illness and complications!
Varicella zoster infection
Varicella-zoster virus causes chickenpox and herpes zoster. The source of infection for chickenpox can only be a person with chickenpox or herpes zoster, including the last 24-48 hours of the incubation period. Convalescent chickenpox remains infectious for 3-5 days after the skin rash stops. The disease cannot be transmitted through a third party. Intrauterine infection with chickenpox is possible in the case of a pregnant woman. Chickenpox can occur at any age, but in modern conditions the maximum number of patients occurs in children aged 2 to 7 years. Herpes zoster develops after primary infection with the Varicella-zoster virus, after the infection passes into a latent form, in which the virus is localized in the spinal, trigeminal, sacral and other nerve ganglia. Endogenous reactivation of the infection is possible.
Possible complications.
More often, the disease passes without dangerous consequences for the patient. But with weak immunity, especially in young children, severe herpes sore throat can lead to serious complications caused by the spread of the virus to other organs:
- serous meningitis
- heart pain, myocarditis
- pyelonephritis
- encephalitis
- conjunctivitis.
To exclude the development of serous meningitis, you need to consult a neurologist; if you have heart complaints, you need to contact a pediatric cardiologist. If there are changes in the general urine test, you must make an appointment with a pediatric nephrologist.
With proper and effective treatment of herpes sore throat complicated by meningitis, the prognosis is usually favorable. But at the same time, the treatment of the youngest patients requires careful attention. With myocarditis the situation is more severe. Any complications of herpetic sore throat require the intervention of specialists!
Acute herpetic stomatitis
Acute herpetic stomatitis is a highly contagious disease of the oral mucosa and gums. It can be considered an independent disease, since the cause is primary infection with the herpes virus. This disease mainly affects children under three to five years of age, who have reduced local (oral mucosa) and general immunity. In older children, the disease appears less frequently (primary infection occurs without symptoms of acute herpetic stomatitis), but even mature people are at risk of this disease in some cases. The incubation period, i.e. the time from infection to the first symptoms ranges from 2-26 days.
Symptoms of acute herpetic stomatitis . The disease begins with a feeling of general malaise. Obvious symptoms of herpes stomatitis appear after a latent period, most often after 10-14 days. Redness of the mucous membrane is observed, small bubbles appear on the tip of the tongue, oral mucosa, gums (at the everyday level they are referred to as herpes on the gums ), and palate. The blisters quickly burst and the formation of lesions is possible - erosions, afts (stage or phase of aphthous stomatitis), ulcers. Additional and concomitant symptoms of herpes stomatitis (acute): pain (even severe) in the oral cavity, increased salivation, bad breath, swelling of the cervical lymph nodes, low-grade fever, headache. In practice, depending on the degree of damage to the mucous membrane and the general condition of the body, there are mild, moderate and severe forms (in childhood, sometimes requiring hospitalization) of acute herpetic stomatitis. Accurate diagnosis is carried out using laboratory tests.
Complications of the disease . In the absence of timely treatment of this disease, dangerous consequences and complications are possible. The disease can unnoticeably progress to chronic recurrent herpetic stomatitis . A herpes infection can spread to the eyes and cause worsening or even loss of vision. The spread of infection to the brain can cause inflammation (encephalitis) with all the ensuing consequences.
Treatment of herpes sore throat in children
There is no specific antiviral treatment. Treatment of the cause of herpetic disease should be carried out according to the following scheme:
- isolation of the patient
- drinking plenty of fluids, bed rest
- actions aimed at relieving and alleviating symptoms.
At the moment, no drug has yet been invented that can kill the causative agent of the disease. You can only alleviate or remove the symptoms. A person recovers completely only when the body develops immunity to the virus. Usually the body takes a week to do this.
First of all, it is advisable to isolate the child from other family members - separate dishes, linen and towels - the disease is contagious. For herpetic sore throat, children are prescribed antihistamines to relieve swelling and irritation. "Claritin", "Suprastin" and others are suitable. To reduce the temperature, use antipyretics: Nurofen, Efferalgan, Paracetamol, etc. To relieve pain in the throat, gargle with decoctions of sage, chamomile, calendula, salt or soda solution. Rinsing should be done every hour. You can use special sprays and aerosols: Hexoral, Ingalipt, Tantum-Verde. Tablets and lozenges relieve pain. It is advisable to use the antiseptic agents Miramistin and Chlorhexidine.
For successful recovery it is necessary to create favorable conditions for the child. It is necessary to provide conditions for sleeping in a well and frequently ventilated room. The diet should consist of soups, purees, and cereals. Food should not be hot so as not to irritate a sore throat. Don't forget about drinking plenty of warm drinks. The patient can be given rosehip decoction, tea with jam or honey.
Note to parents! In case of herpes sore throat, do not inhale, warm up or apply compresses under any circumstances. Such measures will only activate viruses, and the disease will drag on.
Some parents mistakenly lubricate the bubbles in the larynx with iodine or brilliant green. This measure is absolutely ineffective, does not bring any practical benefit, but causes severe pain to the baby.
There is no need to give your child antiherpetic drugs such as Acyclovir and its analogues. As we have already mentioned, the course of the disease has nothing to do with the herpes virus.
Epstein-Barr virus infection
An infectious disease caused by the Epstein-Barr virus (EBV) and characterized by a systemic lymphoproliferative process with a benign or malignant course.
EBV is isolated from the body of a patient or virus carrier with oropharyngeal secretions. Transmission of the infection occurs through airborne droplets through saliva, often when a mother kisses her child, which is why EBV infection is sometimes called the “kissing disease.” Children often become infected with EBV through toys contaminated with the saliva of a sick child or a virus carrier, when using shared utensils and linen. Blood transfusion and sexual transmission of the infection are possible. Cases of vertical transmission of EBV from mother to fetus have been described, suggesting that the virus may be the cause of intrauterine developmental anomalies. Contagiousness during EBV infection is moderate, which is probably due to the low concentration of the virus in saliva. The activation of infection is influenced by factors that reduce general and local immunity. The causative agent of EBV infection has a tropism for the lymphoid-reticular system. The virus penetrates the B-lymphoid tissues of the oropharynx and then spreads throughout the body's lymphatic system. Infection of circulating B lymphocytes occurs. The DNA virus penetrates into the nuclei of cells, while the proteins of the virus give infected B-lymphocytes the ability to continuously multiply, causing the so-called “immortality” of B-lymphocytes. This process is a characteristic feature of all forms of EBV infection.
EBV can cause: infectious mononucleosis, Burkitt's lymphoma, nasopharyngeal carcinoma, chronic active EBV infection, leiomyosarcoma, lymphoid interstitial pneumonia, hairy leukoplakia, non-Hodgkin's lymphoma, congenital EBV infection.
Herpesvirus infection is currently one of the leading medical and social problems not only in Russia, but throughout the world. The variety of clinical manifestations, characteristics of pathogens, almost 100% infection of the population with certain types of herpes, as well as the possibility of spreading the herpes virus through almost all known routes of transmission allowed the WHO Regional Office for Europe to classify herpesvirus infection as a group of diseases that determine the future of infectious pathology.
Herpesvirus infections, or herpetic infections, include infectious diseases caused by a group of human herpes viruses, which are characterized by a variety of clinical forms and tend to be chronic. Predisposing factors for the development of these diseases are often immunodeficiency states [1, 2].
Herpesvirus diseases are an opportunistic infection that develops against the background of immunodeficiency, and their long, recurrent and severe course is regarded by many dermatologists as para-oncological dermatosis or as an AIDS-marker disease [1, 3, 4].
However, difficulties in solving this problem are associated not only with the peculiarities of the course of herpetic infections themselves, but also with the lack of continuity in providing care to patients. Thus, herpetic lesions of the skin and mucous membrane of the oral cavity are treated by dermatologists and dentists, diseases in childhood are observed by infectious disease specialists and pediatricians, genital herpes is dealt with by urologists, gynecologists and venereologists, ophthalmoherpes - by ophthalmologists, damage to the nervous system - by neurologists, damage to the lymphatic system - by hematologists, oncologists, immunologists.
Herpetic infection is one of the very first viral infections that a small child encounters. Unfortunately, it is not possible to prevent children from becoming infected with viruses at such a high level of infection in the population. A large share in the structure of infectious diseases is accounted for by herpes simplex virus (HSV) infection, the clinical manifestations of which in childhood can have significant differences and an unequal prognosis. In most cases, diseases caused by HSV are characterized only by damage to the skin and mucous membranes (dermatological syndrome) and are mild. However, we should not forget that the course and prognosis of herpes infection in children can be different and depend primarily on the state of antiviral immunity. The presence of passive immunity protects most children under 6 months of age from HSV infection and explains the rarity of herpetic diseases in newborns and infants [3].
In childhood, primary infection with HSV is observed, which can manifest not only with skin rashes and damage to the mucous membranes of the oral cavity, genitals, eyes, but also with a pronounced intoxication syndrome, involvement of the central nervous system (CNS) and other organs. The most severe types of HSV infection are combined forms that develop against the background of immunological and/or allergic disorders. In immunodeficiency states (primary or secondary origin), the development of generalized forms of herpetic infection with the risk of death is possible.
Epidemiology of herpes simplex virus
HSV is ubiquitous, highly pathogenic, and causes a wide variety of clinical conditions. There are two types of viruses: herpes simplex virus type 1 (HSV-1) and type 2 (HSV-2). About 80% of initial contacts with HSV (onset of the disease) are asymptomatic. Lesions accompanied by clinical manifestations may differ in severity and variety of symptoms, as well as a high frequency of recurrence. In immunocompromised people, the infection can cause life-threatening conditions [3].
Given the high contagiousness of HSV, infection with the type 1 virus in the vast majority of people occurs in early childhood, after the infant’s passive immunity disappears—maternal antibodies to various infectious agents transmitted transplacentally are destroyed [4]. Most often, children become infected as a result of contact with the saliva of sick parents containing the virus (Fig. 1).
Rice. 1. Residual appearance of labial herpes in the mother and primary infection (Kaposi's eczema) in the child.
A surge in the incidence of HSV-2 is observed in adolescence and adulthood, and detection of this virus in children can be interpreted as an indirect sign of sexual abuse.
HSV can be transmitted directly through close contact with a sick person, as well as sexually and transplacentally. Less commonly observed are airborne, transplantation (during organ transplantation) and transfusion routes of transmission. The incubation period ranges from 3 to 6 days. HSV infection occurs when the virus is inoculated onto the surface of a susceptible mucous membrane (eg, oropharynx, cervix, conjunctiva) or through small skin lesions [4, 5].
The incidence of HSV increases with age and correlates with socioeconomic status, race, and culture. By age 30, 50% of people with high socioeconomic status and 80% with low socioeconomic status are seropositive [6]. A national health survey conducted in the United States [6] revealed HSV-2 seropositivity in 45% of African Americans, 20% of Mexican Americans, and 17% of fair-skinned individuals. It was also noted that seropositivity for HSV-2 is more common in women (25%) than in men (17%). When studying the effect of HSV of various types on the human body, it was noted that antibodies to HSV-1 in patients alleviate the course of the disease caused by HSV-2, and the primary orolabial localization of HSV-1 manifestations protects against genital infection with HSV-1, but not HSV-1. 2 [6, 7].
Clinical manifestations of herpes virus infection in children
Acute herpetic gingivostomatitis
is the most typical manifestation of primary HSV-1 infection, which occurs in children aged 6 months to 5 years. The onset of the disease is acute, the clinical picture is characterized by a violation of the general condition of the child: fever (38-39 ° C), regional lymphadenopathy, anorexia and lethargy. Considering the short incubation period characteristic of HSV, upon examination one can note the presence of signs of the disease in the baby, and residual manifestations of herpes simplex in the parents (hemorrhagic crusts on the lips, wings of the nose, etc.) [8].
Herpetic gingivitis is characterized by swollen, hyperemic, sharply painful “fragile” gums. The vesicles are localized on the mucous membrane of the mouth, tongue and lips, later they quickly open and merge, forming painful erosions covered with a whitish coating. A characteristic sign of herpetic gingivostomatitis is the spread of vesicular-erosive rashes to the mucous membrane of the red border of the lips (Fig. 2).
Rice. 2. Herpetic gingivostomatitis.
The duration of acute herpetic gingivostomatitis is 5-7 days. Virus shedding from saliva can last up to 3 weeks or more. Often, parents “miss” the debut of a herpetic infection, explaining the symptoms of dysphagia and the child’s poor health with teething.
Acute herpetic pharyngotonsillitis
(or herpangina) also refers to frequent clinical manifestations of primary HSV infection. Vesicular elements form erosion-aphthae on the tonsils and posterior wall of the pharynx, covered with a white coating. In school-age children, herpetic pharyngitis and tonsillitis are more common than gingivostomatitis. Characteristic is a combined lesion of the oropharynx and the red border of the lips. You feel unwell: fever, weakness, sore throat. Differential diagnosis is carried out with chronic aphthous stomatitis and damage to the oral mucosa with viral pemphigus caused by Coxsackie enterovirus.
Labial herpes
- the most typical manifestation of a recurrent HSV-1 infection, rashes can be localized not only on the lips, but also on the chin, wings of the nose, periorbital, periauricular, etc. Often manifestations of HSV-1 infection are observed on the skin of the fingers and palms ( especially when saliva gets on injured hands, for example when a child sucks fingers) (Fig. 3) [9].
Rice.
3. Herpetic rashes on the hands of a child. With relapses of herpetic infection in “favorite” places, patients note prodromal sensations of pain, burning and tingling, which are stereotypically felt at the site of further formation of typical herpetic eruptions. The typical form of herpes simplex is characterized by the dynamic development of the elements of the rash: hyperemic papules quickly turn into small thin-walled intraepidermal vesicles, leaving behind erosions. With a long course of the disease (2-3 weeks), the formation of superficial cicatricial atrophy is possible as a result of the disease. A pathognomonic sign of the evolution of herpetic elements is the formation of hemorrhagic crusts, often massive and confluent (Fig. 4).
Rice. 4. Massive hemorrhagic crusts are residual manifestations of labial herpes.
Less commonly, atypical forms of herpes simplex are observed in adolescents. Hemorrhagic-necrotic form
characterized by a large number of grouped vesicles on an edematous hyperemic background.
Some of the vesicles have hemorrhagic contents. When these elements resolve, necrosis and scar formation are observed. Regression of rashes is quite rapid (14-16 days). The edematous form
of herpes simplex often develops in areas of the skin with loose subcutaneous fat (lips, periorbital area, vulva, foreskin).
This form of herpes simplex can lead to the development of persistent swelling, and frequent relapses can lead to the development of elephantiasis-like herpes
.
An impetigo-like form
has been described , reminiscent of streptococcal impetigo in its clinical picture, while rashes in the form of conflicts tend to grow peripherally, and after opening they form massive layered crusts.
Genital herpes
develops in adolescents and young adults soon after the onset of sexual activity. Clinical manifestations of primary genital herpes are more severe in young women. The inflammatory process is characterized by ulcerative or necrotic lesions. Herpetic vesicles are localized on the skin of the external genitalia: labia majora and minora, vestibule and vaginal walls. On the mucous membranes, the blisters quickly open, leaving behind painful ulcers. The vaginal mucosa is inflamed and swollen. The cervix is involved in the inflammatory process in 70-90% of cases. HSV-1 causes urethritis much more often than HSV-2 (Fig. 5, 6).
Rice. 5. Anogenital localization of herpetic rashes in a girl.
Rice.
6. Herpes simplex rash on the buttocks of a boy. In young men, herpetic blisters are localized on the skin of the glans and shaft of the penis, foreskin, and sometimes on the scrotum, inner thighs and buttocks [7].
A rare but extremely severe manifestation of the disease is primary herpes of newborns.
Infection occurs through direct contact of the child with herpetic rashes on the mother during the passage of the birth canal. The risk of infection of a child from a mother with a primary herpes infection is 50% [10, 11]. Primary herpes of newborns is a classic systemic viral disease, often fatal. An unfavorable prognosis is associated with HSV damage to vital internal organs (central nervous system, lungs, etc.). Primary herpes in newborns is characterized by multiple dense vesicular-hemorrhagic rashes on the child's skin; often the mucous membrane of the oral cavity and the conjunctiva of the eyes are involved in the inflammatory process.
An extremely severe form of generalized herpes is herpetic eczema,
or Kaposi's eczema
. The peak incidence in young children occurs between the ages of 8 months and 1.5 years [12]. In children, there is a sharp rise in temperature to 39-40 ° C, a violation of the general condition, and lymphadenopathy. The development of meningeal symptoms, as well as the phenomenon of generalized herpetic infection with the involvement of internal organs in the pathological process, is possible. With recurrent herpetic eczema, in contrast to the primary form, general health is slightly impaired. Rashes in the recurrent form of Kaposi's eczema are localized mainly in places of greatest damage to the skin (for example, the location of herpetic elements in atopic dermatitis on the extensor surfaces of the extremities) (Fig. 7, 8, 9, 10). Often herpetic rashes spread to the periorbital area (Fig. 11). A serious complication in this case is ophthalmoherpes (herpetic conjunctivitis, keratitis, uveitis, chorioretinitis, acute retinal necrosis), which can result in loss of vision [13, 14].
Rice. 7. Severe Kaposi's eczema in an 11-month-old child.
Rice. 8. Vesicular rashes in Kaposi's eczema with umbilical depression.
Rice. 9. Kaposi's eczema.
Rice. 10. Kaposi's eczema.
Rice.
11. Kaposi's eczema. Studies conducted in patients with herpetic eczema that developed against the background of atopic dermatitis confirmed that the greatest risk of this complication is observed in patients with an impaired IFN-γ response [15], with a high level of IgE in the blood serum and polyvalent sensitization [16] . A poor prognostic sign for the development of Kaposi's eczema is also a low level of the antimicrobial peptide cathelicidin peptide LL-37 in the blood [17].
Herpes-associated erythema multiforme exudative (HAMEE) -
a type of infectious-allergic form of exudative erythema multiforme caused by HSV. Erythema multiforme exudative (EME) of herpetic etiology usually develops in adolescents and adult patients, but is not typical for young children [18].
In 95% of patients, GAMEE is combined with orofacial (labial or nasal) localization of herpetic eruptions. The clinical picture of MEE of herpetic etiology is characterized by the appearance of a widespread polymorphic rash on the skin of the trunk and extremities on the 4-6th day from the onset of relapse of herpes simplex. In contrast to the toxic-allergic form of MEE, typical maculopapular target-shaped rashes are characterized by less pronounced exudation, solitary location, stagnant color of the rashes, and relatively small sizes - up to 4 cm in diameter (Fig. 12, 13).
Rice. 12. Residual manifestations on the lips of labial herpes in a teenager with GAMEE.
Rice. 13. Target-shaped maculopapular rash in an adolescent with GAMEE.
The duration of the disease is usually 12-20 days. In some patients, this form may recur several times a year [19].
Researchers have noted that prognostic criteria that increase the risk of developing HAMEE are the presence of the following changes in the immune status of patients with herpes simplex:
- an increase in the spontaneous production of IL-4 and IL-6 in combination with inhibition of their induced production (spontaneous/induced ratio - 1:1);
— in the humoral link there is an imbalance in the synthesis of immunoglobulins with a predominance of IgE and a decrease in IgA with an increase in the absolute content of B-lymphocytes;
- decrease in IFN-α and IFN-γ;
— no increase in NK [20, 21].
One of the hypotheses that explains the occurrence of MEE only in a small number of patients suffering from recurrent herpes is the assumption that the development of HAMEE requires hematogenous spread of HSV - viremia. Recent studies have noted that patients with HAMEE have HSV circulation in affected CD3+, CD4+ cells [22].
Another significant component of the pathogenesis of MEE of herpetic etiology is the development of autoimmune changes in the body: hypersensitivity with an immune complex component of varying severity [23].
Therapy for children suffering from HSV infection
Basic therapeutic measures should be aimed primarily at eliminating the impact of the etiological factor. Causal therapy for herpes simplex is a generally accepted approach to the treatment of acute manifestations of a viral infection and the prevention of its exacerbations and is included in all international standards and recommendations [24, 25]. The main direction of therapy is the use of highly specific antiviral drugs - acyclic nucleosides, which in their chemical structure are modified analogues of the viral DNA component. The first drug was acyclovir. To increase biological activity in the body, acyclovir undergoes three stages of phosphorylation. Acyclovir has specific inhibitory activity against viruses: Herpes simplex
Types 1 and 2,
Varicella zoster
, Epstein-Barr, cytomegalovirus and human herpes virus type 6.
The mechanism of action of acyclovir is associated with inhibition of viral DNA synthesis immediately after phosphorylation of the drug and conversion to the active form - acyclovir triphosphate. The first stage of phosphorylation takes place with the participation of virus-specific enzymes (viral thymidine kinase, which is present in cells affected by the virus). Acyclic nucleosides are most effective when warning signs and/or first symptoms of herpes infection appear. Long-term use of these drugs during the period between relapses serves preventive purposes.
In children, acyclovir is approved for use from birth. Doses of acyclovir are calculated based on 20 mg per 1 kg of body weight in 4-5 doses per day, both parenterally and in tablet form.
The modern second generation acyclic nucleoside is valacyclovir.
(L-valine ester of acyclovir).
Valacyclovir
has a higher bioavailability (54%) and half-life (10-20 hours) compared to acyclovir.
Its effectiveness, high safety profile and ease of use have been repeatedly proven in numerous studies [26, 27]. Valaciclovir
is approved for use
in children over 12 years of age
. Prescription of the drug in adolescents is especially recommended in cases of treatment and prevention of recurrent herpes simplex of various localizations, with herpetic eczema, as well as in complex therapy of GAMEE.
In adolescents, the drug valacyclovir
is prescribed at a dose of 500 mg 2 times a day for a long time (for 7-10 days). The results of treatment of a patient with Kaposi's eczema are presented in Fig. 14 and 15.
Rice. 14. Patient K., 13 years old. Kaposi's eczema that developed against the background of atopic dermatitis - before treatment.
Rice.
15. The same patient. After therapy with valacyclovir 500 mg 2 times a day for 6 days. GAMEE therapy begins with the combined use of steroid hormones and antiviral drugs [28]. All patients are prescribed infusion therapy. Glucocorticosteroids (GCS) are administered parenterally at a dose of 3-5 mg per 1 kg of body weight per day (calculated using prednisolone). The course of therapy with GCS at the indicated dose is 2-4 days, followed by withdrawal within 2-3 days. Valaciclovir
prescribed at a dose of 500 mg 2 times a day for 7-10 days. Long-term prophylactic administration of valacyclovir is recommended for patients who have undergone MEE due to recurrent herpes infection.
Cytomegalovirus infection
Cytomegalovirus infection is characterized by the formation of giant cells and specific infiltrates in the affected organs, a latent (asymptomatic) course in individuals with a normal immune system and with clinical manifestations in immunodeficiency states, mainly in young children.
Clinical forms of cytomegalovirus infection (CMVI):>
Congenital CMV infection is infection from the mother during pregnancy and childbirth and acquired, which is often asymptomatic. The full clinical picture of CMV infection is characterized by:
- increase in body temperature;
- lethargy;
- drowsiness;
- adynamia;
- enlarged lymph nodes, liver, spleen, salivary glands;
- rash;
- other organs are involved (lungs, kidneys, central nervous system).
The disease has an undulating, relapsing course, reminiscent of the clinical picture of infectious mononucleosis.