History of the disease
When collecting anamnesis, it was established that gums have been bleeding when brushing teeth or biting off hard food for several years; the patient does not observe individual oral hygiene (brushing teeth once a day). According to the patient, the last time he visited the dentist was 2 years ago. The patient himself associates severe pain in the gums with a recent flu.
Previous and concomitant diseases
Allergological anamnesis is not burdened. The patient denies the presence of hepatitis, HIV, herpes virus, cardiovascular diseases, disorders of the nervous system, digestive and respiratory systems. As a child, he suffered from acute respiratory diseases. 2 weeks ago I had the flu.
Bad habits - smoking.
Dental treatment is the most widespread type of specialized medical care, which is addressed to patients of all age categories. In industrialized countries in 2000, about 20% of the population was over 60 years of age. According to demographic observations, the proportion of elderly people among the population will continue to grow. 30% of all patients at a dental appointment belong to the anesthetic risk group, that is, they have concomitant diseases [1]. It is also noted that 74% of elderly patients have at least four concomitant diseases, 38% have up to six, and 13% have eight or more [2]. In addition, many patients are sometimes not sufficiently aware of the presence of general somatic diseases, which complicates the assessment of the degree of risk during dental intervention.
The need for dental treatment does not exclude the presence of pathologies in the patient from the cardiovascular, bronchopulmonary, nervous, endocrine, and immune systems; severe damage to the liver, kidneys, as well as elderly and senile age, when compensatory capabilities decrease, which can lead to the development of complications.
Collection of anamnestic data to identify concomitant general somatic pathology
Before providing dental care in an outpatient setting, it is necessary to collect an anamnesis, which is usually carried out in two forms - a questionnaire and a survey. Questioning is convenient to conduct at the pre-medical stage, but it should be noted that a single standard form of questionnaires for collecting anamnesis has not been developed to date.
In questionnaires used within the Russian Federation, the patient is asked to indicate the presence of diseases (Appendix No. 1)
, but the patient may not know that he is sick.
Considering this fact, colleagues from the USA consider it advisable to ask the patient questions in questionnaires about the presence of the most common symptoms of diseases (Appendix No. 2)
. Of course, the use of such questionnaires, due to the large number of questions, significantly increases the time required to collect anamnesis, but makes it possible to identify concomitant diseases in the patient, even if the patient did not know about their presence [3].
The data obtained during the survey must be carefully analyzed by a doctor to conduct a survey, during which additional questions should be asked, according to the diseases indicated by the patient. It should be noted that it is at the interview stage that the “doctor-patient” contact is established.
A thorough history taking allows us to identify concomitant pathologies in the patient, draw up a treatment plan, justify the choice of means and method of pain relief, which will help avoid the development of emergency conditions during a dental appointment.
Content analysis of the drug therapy used by the patient
A large number of concomitant diseases entails taking an equal number of medications—polypharmacy. In modern clinical practice, various combinations of drugs are widely used and the unreasonable simultaneous prescription of more than 5 drugs for the treatment of one disease is one of the problems of modern medicine. Polypharmacy is often the cause of adverse drug interactions. When taking 8 drugs, complications of drug therapy occur in 10% of patients, and when taking 16 - in 40% of patients [4]. An analysis of cases of polypharmacy in Moscow hospitals showed that it occurs in 25% of treatment cases [5].
All pharmacological drugs used by the patient must be included in the medical history. The choice of methods of sedation and local anesthesia is determined based on an analysis of their interaction with the medications that the patient takes in the treatment of concomitant diseases, and the dentist should be interested in the entire list of medications that the patient is currently taking.
Careful collection of anamnesis and analysis of possible negative interactions of medications with painkillers will help to avoid severe general somatic complications during a dental appointment. But it is worth remembering that the patient does not always indicate the presence of previously diagnosed diseases.
When using a local anesthetic solution with a vasoconstrictor (most often epinephrine) in a patient taking beta-blockers, a rise in blood pressure (BP) is possible due to a decrease in the hypotensive effect.
Sympathomimetics weaken the effect of alpha- and beta-blockers (carvedilol, opoxyphenoxymethyl, methyloxadiazole). Drugs from the diuretic group weaken the effect of the vasoconstrictor, which can lead to a decrease in the effectiveness and duration of action of the local anesthetic. With simultaneous use of 1,4-dihydropyridines (nifedipine, nitrendipine, nicardipine, etc.) with sympathomimetics, the antihypertensive effect may be reduced due to sodium retention. When using epinephrine simultaneously with cardiotonic drugs (dopamine, phenylephrine), the risk of arrhythmias increases. It is necessary to take into account the use of antiarrhythmic drugs (digoxin), since adrenergic agonists also increase the likelihood of arrhythmia [6].
Taking various antipsychotics, tranquilizers, hypnotics and anxiolytics by the patient requires careful selection of methods and means for local anesthesia. Thus, droperidol and hydroxyzine reduce the pressor effect of epinephrine, while chlorpromazine enhances the effect of local anesthetics. Flupenthixol, when used simultaneously with epinephrine, can cause a sharp drop in blood pressure [7].
Most anticoagulant drugs do not have a description of their interaction with vasoconstrictors, but the combined use of warfarin with lidocaine increases the risk of bleeding [8].
If the patient is taking anticoagulants, the effect is assessed using the international normalized ratio (INR). If the INR value is less than or equal to 2.0, then dental treatment is possible, but if the INR value is greater than 3.0, consultation with the attending physician is necessary about the possibility of reducing the dose of anticoagulants to achieve values less than 3.0. If the attending physician concludes that changes in the use of anticoagulants are impossible in the acute period of ischemic stroke, then treatment is carried out without reducing the dose, since the risks associated with the possibility of recurrent strokes are much higher than the risks associated with bleeding [9].
Depending on the results of the content analysis, the choice of drugs for sedation and local anesthesia is determined, which will help avoid emergency conditions in an outpatient dental appointment.
Determination of the patient's functional state before dental intervention
Regardless of the presence or absence of concomitant pathology, all patients require an assessment of their functional state on the day of their visit to the dentist, which includes a rapid assessment of blood pressure and determination of heart rate (HR).
Method for determining blood pressure
In order to determine blood pressure and heart rate using the simplest and most accessible auscultatory method according to N.S. Korotkov, the dentist will need no more than 5 minutes. The use of automated (auscultatory or oscillometric) devices is allowed, but only in cases where their accuracy in clinical practice is confirmed in special studies [10]. In modern clinics, such devices are installed in the examination room or at the entrance to the clinic. The results obtained can be entered into the medical history. For patients whose blood pressure levels exceed the norm, planned dental treatment is recommended to be postponed, and emergency dental care is recommended to be provided after blood pressure correction [6, 11].
A study to identify the incidence of patients with arterial hypertension at an outpatient dental appointment, including 1590 patients aged 18 to 85 years (730 men and 860 women), showed that at a dental surgical appointment, systolic blood pressure (SBP) ≥140 mmHg. Art. and diastolic blood pressure (DBP) ≥90 mmHg. occur in 75% of patients (Fig. 1) [12]. At a therapeutic appointment before routine dental care, SBP readings≥140 mmHg. and DBP ≥90 mm Hg. were noted in 34.6% of patients, and before emergency dental intervention, an increase in blood pressure levels was recorded in 65.9% of patients. At an orthopedic dental appointment, an increase in blood pressure was detected in 29.5% of patients.
Rice. 1. Percentage of patients with SBP≥140 mmHg. and DBP ≥90 mm Hg. when providing various types of outpatient dental care.
Heart rate determination
Determination of heart rate is carried out by assessing the pulsation on the radial artery of the left hand with the tips of the II, III and IV fingers, covering the patient’s hand in the area of the wrist joint with the right hand. After detecting a pulsating radial artery, the properties of the arterial pulse are determined: frequency of beats per minute, rhythm, tension, filling, magnitude. A pulse rate of less than 60 beats per minute is considered bradycardia, and a pulse rate of 80 to 120 beats per minute is considered tachycardia.
For patients suffering from diabetes, the protocol for assessing their physical condition on an outpatient basis includes determining the level of glucose and glycated hemoglobin in the blood using various devices that can be either in the clinic or with the patient.
If the patient is taking anticoagulants, then before dental surgery it is also recommended to determine INR values in an outpatient dental appointment using special devices.
Thus, in order to prevent emergency conditions before a dental appointment, a mandatory condition is to determine the patient’s functional state.
Monitoring hemodynamic parameters
During dental interventions in patients with concomitant pathologies, monitoring of hemodynamic parameters is recommended. For this purpose, we use a pulse oximeter to record heart rate, a tonometer to measure blood pressure (Fig. 2), and, if available in the clinic, a separate monitor with registration of all hemodynamic parameters, intended for anesthesia (Fig. 3).
Rice. 2. Measuring blood pressure with a mechanical tonometer.
Rice. 3. Monitoring of hemodynamic parameters during the provision of dental care in an outpatient setting.
ASA Anesthetic Risk Classification
When treating patients with general somatic pathology, the dentist does not have any difficulties using various modern technologies, but questions arise about the safety of providing outpatient care.
In patients with a history of a risk factor, the dentist determines the need for consultation with the attending physician (therapist, immunologist, etc.) and further examination. Based on the data received from specialists, the dentist decides on the location of dental care (in a multidisciplinary or specialized hospital or in an outpatient dental facility), based on the international classification of anesthetic risk ASA, which distinguishes 5 classes of the physical condition of patients. This classification is adapted to dental practice by Professor S.F. Malamed and is widely used in world practice [13].
On an outpatient basis, it is possible to receive patients of classes I and II. Class III patients can be admitted on an outpatient basis only with the permission of the attending physician and/or after consultation with an anesthesiologist. If care is provided on an outpatient basis, then the presence of an anesthesiologist is necessary [12].
2) External examination of the maxillofacial area
Pale skin. The facial configuration has not been changed. Turgor is normal. No seals were found. The red border of the lips has a clear border.
The submandibular lymph nodes are enlarged, painful on palpation, and not fused with the underlying tissues. Bad breath (halitosis) is detected.
Facial examination:
the face is symmetrical, the height of the lower third of the face corresponds to the norm, the line of lip closure is normal, the mouth gap is of normal size, the chin and nasolabial folds are not pronounced, the lower jaw is in a state of physiological rest. The corners of the mouth are without pathological changes.
When palpating the TMJ, no crunching, painful sensations, or clicks were detected. ulcerative necrotizing gingivitis diagnosis
Examination of the vestibule of the oral cavity
By measuring the distance from the neck of the teeth to the transitional fold, the depth of the vestibule of the oral cavity is normal. When the lips are abducted, ischemia and blanching of the gum areas are not observed.
Examination of the oral cavity itself:
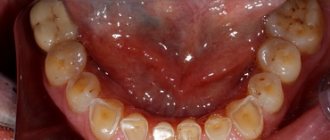
When examining the oral cavity, a large amount of microbial plaque on the teeth, food debris, tartar deposits, and carious cavities are noted.
The interdental papillae and marginal gums are covered with a grayish necrotic plaque, which is easily removed, revealing a moist bleeding surface. The tongue is covered with a grayish-white coating.