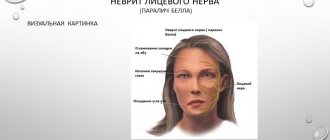
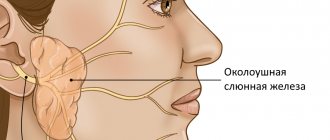
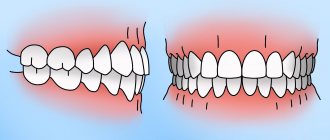
Osteosynthesis of the jaw is a method of surgical treatment of bone fractures using special, most often metal, structures. Osteosynthesis surgery is performed if the fracture site cannot be secured with splints, and also when it is difficult to fix bone fragments. There are different methods of performing the operation, they can be used depending on the type of injury and its severity.
Osteosynthesis allows you to maintain the required level of blood circulation in the damaged bone, which means that such a fracture will heal faster. Not only the integrity of the bone is restored, but also its structure, and this will take only a few weeks.
During the rehabilitation period, it is important to follow certain rules and monitor your well-being and the condition of your bone tissue. Violations of doctor's instructions can lead to pain and even loss of chewing functions.
Indications for osteosynthesis
Osteosynthesis may be prescribed in the following cases:
- if there are not enough stable molars at the fracture sites;
- upon impact, the fragments moved significantly;
- broken jaw bone behind teeth. With such an injury, individual parts of the bone tissue are displaced;
- the injury occurred as a result of the development of inflammatory diseases that thin the bone tissue;
- in case of a fracture of the lower jaw, if too small or massive fragments have formed;
- if the branches and body of the jaw are incorrectly positioned relative to each other;
- it is necessary to perform reconstructive surgery or osteoplasty.
Discussion
Despite the development of medicine in general and maxillofacial surgery in particular, the problem of providing emergency medical care for fractures of the facial skull remains not fully resolved. Due to the increase in the number of road traffic accidents and domestic conflicts, and the passion of young people for traumatic sports, there has been an increase in the number of victims with injuries to the facial skull, among which fractures of the lower jaw occupy the first place [12].
The difficulty of early diagnosis of fractures of the angle of the mandible is associated with the insufficient information content of routine methods of radiation examination (radiography of the skull in frontal or lateral projection), late referral of victims to specialized maxillofacial hospitals and, as a consequence, the choice of irrational methods of treatment, which in turn leads to development of various kinds of complications, reduction in the quality of treatment and life of patients.
Types of osteosynthesis
There are several methods of osteosynthesis; the doctor decides what type of operation the patient needs. Most often, surgeons combine several methods with each other to achieve better results.
Osteosynthesis of the jaw can be:
- Open. It is usually used for severe fractures. During the operation, soft tissue is cut and bone fragments are exposed. They are connected to each other and non-functional small fragments are removed, compressed soft tissues and fascia are released. However, with such an operation, there is still the possibility of tissue peeling off from the bone, then the callus at the fracture site will not be formed correctly. And this can affect the patient’s quality of life. In addition, stitches remain on the skin and paresis (decreased activity) of facial muscles is even possible. Depending on the type of fastening device, it is possible that the incision on the face will have to be made again to remove the fastener.
- Closed. The doctor combines bone fragments without cutting facial tissue;
- Focal. The fixing fastener is applied directly to the fracture site;
- Extrafocal. Fasteners are placed on top of the skin, above the fracture site.
The essence of osteosynthesis and what kind of procedure it is
With osteosynthesis, the doctor not only connects the fragments of the damaged jaw, but also securely fastens them with metal structures or glue.
Open focal osteosynthesis is carried out using:
- Bone suture. If the lower jaw or cheekbone is broken and the injury is recent, it can be fastened with a bone suture. For this, stainless steel, titanium wire or nylon thread is used.
During the operation, the doctor dissects the soft tissues of the face and fixes the fragments with wire. If the fragments are connected using a bone suture, the patient retains chewing function and can continue to care for the oral cavity. This method is contraindicated if the fracture site is inflamed or the patient has an infectious or purulent bone lesion.
- Installation of periosteal metal mini-plates. This method has proven itself in the treatment of all types of jaw bone fractures, except those in which a large number of fragments have formed. In this case, it is enough to make an incision only on one side. The doctor aligns the fracture sites, applies mini-plates to them and screws them on. Nowadays, mini-plates are most often fixed inside the oral cavity.
- Fixation with quick-hardening plastics. It is practiced only for fractures of the lower jaw. After exposing the bone fragments, the doctor makes a bone groove and places a special fixing compound in it. Excess plastic is removed with a cutter, after which the wound can be sutured.
- Osteoplast glue. This composition for fixing bone fragments is made of purified epoxy resin with an organic antiseptic - resorcinol. After application, the glue hardens in 8-12 minutes and reliably fixes the combined bone fragments. Nowadays this method is rarely used.
- Metal staples. For osteosynthesis, staples made of nickel-titanium alloy are used. At low temperatures, the alloy becomes plastic and is easy to shape into the desired shape. Then, at room temperature, the staple regains its previous shape. During the operation, it is first cooled, then inserted into the prepared holes on the bone fragments. As soon as the staples warm up, they straighten and securely fix the fracture site. Metal staples are especially convenient for fixing a fracture of the angle of the lower jaw.
Closed focal osteosynthesis is practiced for healing fracture sites where bone displacement has not occurred. Methods:
- Installation of Kirschner spokes. The doctor inserts metal needles into the bone fragments using a surgical drill. For reliable fixation, the needles are fixed into each fragment to a depth of up to 3 cm. There is no need to dissect soft tissues; the operation is performed through the mouth. This is a low-traumatic practice, but wearing needles creates a lot of inconvenience for the patient.
- Applying a surrounding suture. Applicable when the fracture gap is displaced forward or backward along the jaw. In this case, the suture passes through the central part of each bone fragment. If there are a lot of fragments, the operation takes a long time, but this is one of the most reliable methods of osteosynthesis. It allows the patient’s jaws to be restored even after very complex injuries.
Introduction
Injuries to the maxillofacial region continue to remain one of the pressing surgical problems, which is associated with an increase in the number of patients with fractures of the facial skull bones as a result of road accidents and domestic conflicts, the aggravation of this type of pathology, and the increase in multiple and combined injuries [1, 2]. According to specialized literature, the share of maxillofacial trauma in the structure of various injuries among the urban population is 3.2–8.0% [3]. Fractures of the lower jaw account for up to 85% of the total number of fractures of the facial skull [4–7]. The development and implementation of new methods for fixing bone fragments have significantly increased the effectiveness of surgical treatment in the category of patients under discussion; however, according to a number of authors, complications range from 5.2 to 38.4% of cases [8–11].
Many of the proposed methods are successfully used in everyday practice for performing osteosynthesis for facial skull fractures - titanium plates on the bone, bone suture with stainless steel or tantalum wire, Kirschner wires, a possible combination of bone suture and wires, fixing structures made of shape memory materials. The purpose of this article is to describe the clinical use of titanium nickelide (nitinol) shape memory brackets for mandibular angular fractures.
Clinical case
Patient T.
, 41 years old, was admitted to the clinic of maxillofacial surgery of the University Clinical Hospital (UCH) No. 2 of the First Moscow State Medical University named after. THEM. Sechenov with complaints of pain in the lower jaw on the right, aggravated by chewing and opening the mouth, swelling of the face on the right, and malocclusion.
From the anamnesis it was established that the injury was received as a result of a fight with an unknown person 8 hours before going to the hospital. The patient did not report any compression phenomena. He went to the trauma center, where an X-ray of the skull and intermaxillary fixation were performed using Tigerstedt dental splints. The patient was taken by an ambulance team to the clinic of Clinical Hospital No. 2 of the First Moscow State Medical University named after. THEM. Sechenov, was hospitalized on an emergency basis.
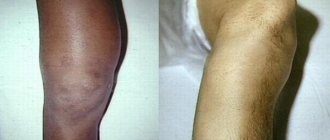
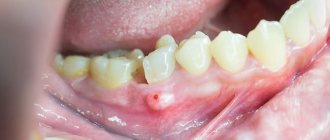
On admission: general condition is relatively satisfactory. Somatic status without features. Upon examination, pronounced swelling of the soft tissues in the parotid-masticatory, buccal and submandibular areas on the right was determined. It was difficult to gather the skin into a fold; local pain was noted on palpation. Regional lymph nodes are not enlarged. The symptom of direct and indirect load is positive in the area of the angle of the lower jaw on the right. Vincent's sign was positive on the right side. From the side of the oral cavity: opening is limited to 2 cm, there was a violation of the closure of teeth such as an open bite on the right. Ruptures in the mucous membrane of the alveolar part of the lower jaw in the area of 4.7–4.8 teeth, as well as the presence of hemorrhagic clots in the oral cavity, were visualized. Swallowing is free, moderately painful (Fig. 1, 2,
Rice. 1. Patient T.’s appearance during hospitalization.
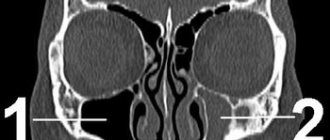
Rice. 2. Orthopantomogram of patient T. during hospitalization. There is a violation of the integrity of the bone tissue in the area of the angle of the lower jaw on the right with the presence of tooth 4.8 in the fracture line. 3).
Rice. 3. X-ray of the skull of patient T. in a direct projection.
Based on complaints, anamnesis, clinical examination and x-ray examination, the diagnosis was made: “Fracture of the lower jaw in the area of the angle on the right with displacement of fragments.”
After additional examination and preoperative preparation, on the day of admission to the hospital, the patient underwent surgical intervention: osteosynthesis of the lower jaw in the area of the right angle using external access using titanium nickelide brackets.
The operation was performed as follows: with premedication under local anesthesia with Sol. Lidocaini 1% 20 ml, on the side of the fracture parallel to the edge of the lower jaw, retreating 2 cm in the area of the angle, a skin incision 4 cm long was made. The skin, subcutaneous fat, superficial fascia of the neck and m. Platisma. The masticatory muscle itself was cut off at the point of attachment to the angle of the lower jaw. The lower jaw in the area of the angle is skeletonized. After visualization of the fracture line, small bone fragments were removed, soft tissue interposition was eliminated, and blood clots were removed. Before performing osteosynthesis of the lower jaw, a loose bone fragment and tooth 4.8 were removed from the fracture line (Fig. 4),
Rice. 4. A removed bone fragment not connected to the periosteum, and tooth 4.8 from the fracture line. Reposition of bone fragments was performed. The bite was fixed in the patient’s usual position using rubber rods and osteosynthesis was performed using two Ω- and S-shaped titanium nickelide brackets under bite control (Fig. 5).
Rice. 5. Operation stage. Osteosynthesis of the lower jaw using Ω- and S-shaped titanium nickelide brackets.
The brackets were installed as follows: holes were formed bicortically on each fragment using a drill, then the legs of the bracket, pre-cooled to +1-3 °C, were bent to the sides (the bracket was activated) and inserted into the corresponding milling holes. When the bracket was heated to 35-36 °C, the original shape was restored - the legs of the bracket were brought closer together, which led to dosed compression of the bone fragments. The postoperative wound was treated with antiseptic solutions, and a latex graduate was installed. The wound was sutured in layers. Hemostasis was performed during the operation.
The postoperative period was uneventful. The patient was discharged for outpatient observation on the 7th day after surgery, after removal of the sutures. Mouth opening at the time of discharge was 3.0 cm.
On the 2nd day after surgery, control radiographs of the skull in a direct projection and orthopantomography were performed. The position of the bone fragments and fixation structures was correct, no secondary displacements were detected (Fig. 6,
Rice. 6. Orthopantomogram of patient T. after surgical treatment. 7).
Rice. 7. X-ray of the skull of patient T. in a direct projection after surgical treatment.
During a follow-up examination after 1 month, an increase in mouth opening to 4.2 cm was noted; the patient’s chewing function and appearance were completely restored (Fig. 8).
Rice. 8. a — appearance of patient T. 1 month after surgery; b — amplitude of mouth opening of patient T. 1 month after surgery. As a result of dynamic observation and interdisciplinary treatment together with a physiotherapist, the prescription of physiotherapy and vitamin therapy on the affected side, the sensitivity of the skin and teeth in the zone of innervation of the inferior alveolar nerve was restored after 6 months.
Over a three-year observation period with examinations once every 6 months, a stable state of occlusion, absence of pain in the lower jaw and neuropathy of the inferior alveolar nerve were noted.
Osteosynthesis using ultrasound
With the help of metal fasteners, the jaw bones can be fixed quite firmly. But during surgery, it is most often necessary to cut through facial tissue and the salivary glands or branches of the facial nerve can be damaged.
It is less traumatic to perform osteosynthesis using ultrasound. In this case, the bone-fixing devices can be inserted shallowly into the bone and a small amount of scars remains on the patient’s face.
The doctor uses low-frequency ultrasound on a titanium plate with spikes. A plate with holes for the dental bur is placed at the fracture site and adapted to the shape of the jaw. An instrument is then used to make shallow holes in the bone through the plate. After which low-frequency ultrasound vibrations are directed to the base of the spines. In this way, the spikes gradually sink into the bone tissue, reliably fixing bone fragments. In this case, an antiseptic solution is supplied through the instrument, which treats the wound.
The bone tissue around the spines becomes denser under the influence of ultrasound. This occurs due to the large contact area, reducing pressure on the bone due to the use of a spike and the internal compression force of the bone tissue.
Ultrasonic osteosynthesis can reduce the time of surgery and reduce the amount of postoperative trauma. The method gives fewer complications and provides a good cosmetic effect.
Compression-distraction osteosynthesis of facial bones in children
Currently, the number of children with congenital and acquired defects and deformities of the maxillofacial area has increased. In this case, vital functions such as breathing, vision, chewing, swallowing, and speech are disrupted. With severe underdevelopment of the lower jaw in children, the root of the tongue moves posteriorly and narrows the lumen of the upper respiratory tract, resulting in breathing problems, more often during sleep, which can lead to the death of the child. Children with cosmetic defects become shy, depressed, secretive, and uncommunicative. In addition, serious mental suffering leads to their aggressiveness and bitterness. Underdevelopment and defects of individual facial bones that are not corrected in childhood cause gross secondary deformations, which are not always and are difficult to correct at an older age.
Today, there is no single surgical treatment method that can reliably eliminate various facial deformities associated with underdevelopment and defects of the skull bones. Osteoplastic operations performed using various types of grafts, titanium plates, biocomposites, silicone are not reliable enough in eliminating deformations, defects and underdevelopment of the bones of the facial skeleton and are often unacceptable for children of different ages. With the simultaneous movement of the bones of the midface, in addition to relapses, more severe complications arise: significant profuse bleeding, partial necrosis of bone fragments and even deaths.
In the last decade, the method of compression-distraction osteosynthesis (CDO) in the maxillofacial area has been intensively developed in the world, since this method does not lead to the development of complications that arise when performing bone grafting (Habal MB, 1995; McCormick SU, 1995; Cohen SR, 1995; Polley J., 1995; Mo na ste rio O., Mo li na F., 1997; Klein C., 1998; Boz zet ti
A. et al., 2001; Mi no ru U., 2001; Moli na F., 2004; Ha ra da K., 2007).
To date, quite a lot of treatment methods and compression-distraction devices (CDAs) have been developed for children with underdevelopment and defects of the lower jaw (Roginsky V.V. et al., 2001, 2002, 2007).
In 1954 G.A. Ilizarov proposed a method for treating patients with various congenital and acquired deformities of long bones.
Carrying out EDT is possible only with the use of CDA. The bulkiness of domestic distraction devices and the complexity of their manufacture have led to the fact that in our country CDO has not received proper development, as a result, for many years, thousands of patients have not received high-quality, comprehensive treatment. The lag behind Western countries, despite the domestic priority of KW, was 20-30 years. The need for this type of help among Moscow children alone is about 500 people a year, and in Russia as a whole it is several hundred thousand people.
Despite the fact that CDO is successfully used all over the world to treat adult patients, many important unresolved issues remain regarding the treatment of children: the distraction mode depending on the pathology zone; age at which this method can be used; the need to develop the most
gentle methods of surgical interventions to individual areas of the facial skeleton; lack of clear indications and contraindications for the use of the method and the use of various types of CDA. In addition, it is still not clear how CDA affects the morphogenesis of tissues of the maxillofacial region in children during their growth; the most reliable and easy-to-use CDA, which can reduce the percentage of complications, have not been developed.
Indications for the use of medical technology
Using KDO on the lower jaw:
1. Underdevelopment of the branch and/or body of the lower jaw, accompanied by disocclusion.
2. Defect of the body or branch of the lower jaw.
3. Respiratory obstruction syndrome, as a consequence of severe underdevelopment of the lower jaw.
4. Combined underdevelopment of the lower and upper jaws.
5. Underdevelopment of the chin of the lower jaw.
Using KDO on the upper jaw:
1. Upper retromicrognathia.
2. Facial deformation in the frontal region of the upper jaw.
Using KDO on the middle zone of the face:
1. Exophthalmos, as a consequence of underdevelopment of the zygomatic-orbital complex.
Contraindications to the use of medical technology
1. Allergic reactions to metal.
2. Osteoporosis.
3. Severe mental disorders.
Logistics support for medical technology
1. A set of titanium assemblies and parts for assembling intraoral compression-distraction devices for the correction of congenital and acquired defects and deformations of the upper and lower jaws and instruments for installing NUD-KD/TMJ - “Konmet” (Russia). Registration certificate FS No. 022a4337/098704 dated December 20, 2004
2. A set of titanium components and parts for assembling external fixation and distraction devices for fractures and deformations of the lower jaw, instruments and devices for their installation, NUD-FD/NC - “Konmet” (Russia). Registration certificate FS No. 022a4339/0988-04 dated December 20, 2004
3. A set of titanium components and parts for assembling distraction external fixation devices for fractures of the bones of the midface and upper jaw and tools for their installation, NE-D/SZVCH - “Konmet” (Russia). Registration certificate FS No. 022a4338/0989-04 dated December 20, 2004
Description of medical technology
A method for eliminating underdevelopment and/or defect of the lower jaw, combined with underdevelopment of the upper jaw (RF Patent for invention No. 2267303).
Preparing patients for planned surgery is carried out according to general rules: general blood test with hemosyndrome, blood group and Rh factor, biochemical blood test, general urinalysis, electrocardiogram. The main stages of the preoperative examination are X-ray (teleradiograms in two projections, orthopantomogram, computed tomography), cephalometry, photo documentation.
The operation is performed under endotracheal anesthesia. Using an incision up to 6 cm in the oral cavity along the transitional fold on the affected side, the branch of the lower jaw is skeletonized. The osteotomy line is marked: the outer cortical layer is sawed with a bur or saw, and the outer and inner cortical plates are sawed along the anterior and posterior edges of the lower jaw branch (the inner cortical plate in the middle part is preserved). An intraoral on-bone CDA is installed, previously untwisted by 2 - 3 mm, so that compression can subsequently be carried out. Using a drill with a diameter of 1.6 mm, create holes for the screws. Holes are drilled through 2 cortical layers. The depth gauge determines the length of the holes. Based on this, self-tapping screws of the required length with a diameter of 2 mm are selected. The device is fixed to the bone fragments so that the screws pass through 2 cortical layers. The screws are tightened until they stop. An osteotome is used to break the inner cortical plate. Compression of bone fragments is carried out. Hemostasis is carried out during the operation. The wound is sutured in layers.
Then an incision is made along the transitional fold from the tubercle of the upper jaw on one side to the tubercle of the opposite side. The upper jaw is skeletonized on both sides. An intraoral to bone KDA is fixed to the upper jaw on the affected side with at least 12 screws with a diameter of 2 mm and a length of no more than 5-7 mm. The device is fixed at an angle to the midline so that during distraction it ensures the divergence of bone fragments in the form of a wedge, the apex of which is located in the area of the zygomaticalveolar crest of the healthy side. An osteotomy of the vomer, as well as the upper jaw, is performed at the level of the pyriform foramina on both sides with an osteotomy in the area of the pterygomaxillary joint on the healthy and affected side (Fig. 1). Compression is in progress. Hemostasis is carried out during the operation. The wound is sutured in layers.
Rice. 1. Schemes of the developed technique: a - operation; b - the result obtained.
In the postoperative period, antibacterial therapy, rinsing the mouth with an antiseptic solution, and daily change of aseptic dressings are carried out. Distraction of the lower jaw begins on the 5th day after surgery, 1 mm per day in 4 doses of 0.25 mm; distraction of the upper jaw - on the 10th day, 0.5 mm per day in 2 doses of 0.25 mm. The retention period lasts at least 12 weeks.
Method for eliminating underdevelopment of the chin of the lower jaw (RF Patent for invention No. 2268016).
Preparing patients for a planned operation is carried out according to general rules: general blood test with hemosyndrome, blood group and Rh factor, biochemical blood test, general urinalysis, electrocardiogram. The main stages of the preoperative examination are X-ray (teleradiograms in two projections, orthopantomogram, computed tomography), cephalometry, photo documentation.
The operation is performed under endotracheal anesthesia. Using an incision in the oral cavity along the transitional fold from the retromolar region of one side to the retromolar region of the other side, the body of the lower jaw is skeletonized on both sides. The neurovascular bundle is carefully mobilized on both sides. In the area of the angle of the lower jaw, a CDA is installed parallel to the lower edge of the body, previously untwisted by 1-2 mm, so that compression can subsequently be carried out. Using a drill with a diameter of 1.6 mm, create holes for the screws. Holes are drilled through 2 cortical layers. The depth gauge determines the length of the holes. Taking this into account, self-tapping screws of the required length with a diameter of 2 mm are selected. The device is fixed to the bone fragments with 6 screws so that the latter pass through 2 cortical layers. The screws are tightened until they stop. The device screw is brought out through a separate incision
(0.3 mm) on the skin in the area behind the ear. In a similar way, the second KDA is fixed in the area of the angle of the lower jaw on the other side. Using an oscillating saw, an extended osteotomy of the mental region is performed: after the mental region, the osteotomy line goes through the body to the angle of the lower jaw on both sides. The osteotomy line passes below the roots and buds of the teeth. Compression of the bone fragments is performed (Fig. 2). Hemostasis is carried out during the operation. The wound is sutured. A suture is placed on the wound in the area where the screw of the device comes out on the skin.
Rice. 2. Schemes of the developed method: a - operation; b - the result obtained.
In the postoperative period, antibacterial therapy, rinsing the mouth with an antiseptic solution, and daily change of aseptic dressings are carried out.
Distraction begins on the 5th day after surgery, 0.5 mm per day in 2 doses of 0.25 mm. The retention period lasts at least 12 weeks.
Method for simultaneous elimination of underdevelopment of the branch and body of the lower jaw
Patients are prepared for planned surgery according to general rules: general blood test with hemosyndrome, blood group and Rh factor, biochemical blood test, general urinalysis, electrocardiogram. The main stages of the preoperative examination: X-ray (teleradiograms in two projections, orthopantomogram, computed tomography), cephalometry, photo documentation.
The operation is performed under endotracheal anesthesia. The lower jaw is skeletonized using an incision of up to 6 cm in the submandibular region on the affected side. An osteotomy line is marked in the area of the branch and body: the outer cortical layer is sawed with a bur or saw, and along the anterior and posterior edges of the lower branch
the jaws saw through the outer and inner cortical plates (the inner cortical plate in the middle part is preserved). The bone-mounted CDAs are installed, previously untwisted by 2 - 3 mm, so that compression can be carried out subsequently. Apparatus in the region of the mandibular ramus
installed parallel to its posterior edge, and on the body - parallel to the occlusal plane; in addition, the screw of the device is brought out through a separate incision (0.3 mm) on the skin in the area behind the ear. Using a drill with a diameter of 1.6 mm, create holes for the screws. Holes are drilled through 2 cortical layers. The depth gauge determines the length of the holes. Taking this into account, self-tapping screws of the required length with a diameter of 2 mm are selected. The devices are fixed to the bone fragments so that the screws
pass through 2 cortical layers. The screws are tightened until they stop. An osteotome is used to break the inner cortical plate. Compression of bone fragments is performed. Hemostasis is carried out during the operation. The wound is sutured layer by layer (Fig. 3).
Rice. 3. Scheme of the developed method: a - operation; b - the result obtained.
Antibacterial therapy and daily change of aseptic dressings are carried out in the postoperative period.
Distraction begins on the 5th day after surgery, 1 mm per day in 4 doses of 0.25 mm. The retention period is at least 12 weeks.
Elimination of underdevelopment of the middle zone of the face
Preparing patients for a planned operation is carried out according to general rules: complete blood count with hemosyndrome, blood group and Rh factor, biochemical blood test, general analysis
urine, electrocardiogram. The main stages of the preoperative examination are x-ray (teleradiograms in two projections, orthopantomogram, computer tomography).
mography), cephalometry, photo documentation.
The operation is performed under endotracheal anesthesia. Before the operation, boys are shaved bald, and girls have their hair shaved in the form of a path about 4 cm wide along the intended incision. Bilateral transvenous access is used. The cut line is wavy. Before the incision, hydropreparation of the tissue is carried out. The frontal bone is skeletonized so that the periosteum remains 2 cm before the upper edge of the orbits. The temporal and infratemporal fossa are separated from the muscles on both sides. Skeletonizes the root of the nose and nasal bones. Very carefully, the roof and bottom of the orbits are isolated. When skeletonizing the medial walls of the orbits, the nasolacrimal canal is carefully isolated, and a ligature is also applied in the area of the canthal ligaments in order to fix them in the right place when suturing the wound. WITH
using an oscillating saw, an osteotomy is performed along the line of the frontonasal suture, continuing the osteotomy line down through the bony part of the nasolacrimal canal (without damaging the soft tissue part
channel), the bottom of the orbit. Next, the cut is carried out upward, along the lateral edge of the orbit and ends at the level of the frontozygomatic suture. Also, using an oscillating saw, an osteotomy of the zygomatic arch is performed closer to the zygomatic bone in its widest part. Then, using 3 small incisions in the oral cavity along the transitional fold of the upper jaw, access is made to the vomer and pterygomaxillary joints. An osteotomy of the vomer is also performed in the area of the pterygomaxillary joint on both sides. Using a curved chisel, an osteotomy is performed in the area of the nasal root along the vertical plate of the ethmoid bone and the vomer. At this point, you must be extremely careful not to damage the endotracheal tube. Once all cuts have been made, the midfacial complex is mobilized using Rowe forceps.
The bone apparatus is fixed with self-tapping screws to the zygomatic and parietal bones. When fixing to the zygomatic bone, screws with a diameter of 2 mm and a length of 7 mm are used, and when fixing to the parietal bone, screws with a diameter of 2 mm and a length of 5 mm are used. After fixing the devices, compression is performed. It is important to note that the devices are installed parallel to the zygomatic arches. Careful hemostasis is carried out throughout the entire operation. The wound is sutured in layers.
In the postoperative period, antibacterial therapy, thorough oral hygiene and daily change of aseptic dressings are carried out.
Distraction begins on the 7th day after surgery, 1 mm per day in 4 doses of 0.25 mm. After the required functional and cosmetic result is achieved, the distraction is stopped. The duration of the retention period is on average 12 weeks.
Possible complications when using medical technology and ways to eliminate them
1. Lack of bone regenerate. Individual rhythm and tempo of distraction, repeated distraction.
2. Osteomyelitis or inflammation of soft tissue in the area of the device, sinusitis. Compliance with the rules of asepsis and antisepsis, antibacterial therapy, early removal of the device.
3. Device breakdown. Replacing the device. Repeated distraction.
4. Incorrect vector of distraction and, as a consequence, a violation of facial aesthetics or a discrepancy between the functional result and the expected one. Repeated corrective surgery.
Effectiveness of the use of medical technology
The EDC method was used in 198 patients with underdevelopment and/or defects of various congenital and acquired skull bones aged from 14 days to 17 years. Of these, 156 children had underdevelopment and/or defects of the lower jaw of a congenital or acquired nature; with underdevelopment of the upper jaw after cheilouranoplasty for congenital unilateral cleft of the upper lip, alveolar process and palate - 16; with underdevelopment of the upper jaw after cheilouranoplasty for congenital bilateral cleft of the upper lip, alveolar process and palate - 12 children; with Binder syndrome - 2; with Crouzon syndrome - 10; with Apert syndrome - 1 child; with plagiocephaly - 1 patient. The operations were performed according to vital, functional and cosmetic indications.
As a result of applying the EDC method, the following results were obtained: good - in 77.3%, satisfactory - in 13.6% of patients and negative - in 9.1% of children (Fig. 4). With good and
In satisfactory results, the length of the bone regenerate was 10 - 40 mm.
Rice. 4. Diagram of the obtained results.
During lengthening of the mandibular ramus without distraction of the upper jaw, an open bite is formed on the affected side from 7 to 12 mm.
After removal of the CDA, after 1 month, the open bite is not determined, which is not due to the growth of the upper jaw, as was previously thought, but to the reduction of the regenerate due to the action of the masticatory muscles. The size of the reduction is 40-50% of the original length. So, to avoid this type
complications, it is necessary to simultaneously lengthen the branch of the lower jaw with the upper jaw. The need for distraction of the upper jaw with congenital pathology is 75%, and with acquired pathology - 30%.
The proposed method for simultaneous elimination of underdevelopment of the lower and upper jaws has the following advantages:
— the age limit has been significantly reduced, the method can be used from 1.5 years;
— there is no intermaxillary fixation;
— the function of the upper and lower jaws is preserved, which has a positive effect on the formation of the regenerate;
— the possibility of nutritious nutrition and adequate oral care;
— acceptable appearance of the patient;
— there are no postoperative scars on the skin;
— unlimited retention period;
— the risk of developing inflammatory processes is significantly reduced;
— the possibility of performing independent distraction of the upper and lower jaws with an individual distraction schedule for each jaw.
In children with bilateral underdevelopment and/or a defect of the lower jaw, congenital or acquired, underdevelopment of the chin is always determined, especially for patients with Treacher-Collins syndrome and patients who have long suffered from bilateral ankylosing lesions of the temporomandibular joint. After eliminating bilateral underdevelopment or defect of the lower jaw and restoring a constructive bite, about 70% of children require surgical correction of the chin.
Numerous methods of genioplasty are known using autografts, allografts, and plastic surgery using endoprostheses made of various synthetic materials (EGMASS-12, silicone, PolyGap).
The method for eliminating underdevelopment of the chin of the lower jaw has the following advantages:
— the age limit has been significantly reduced, the method can be used from 5-6 years;
— absence of possible negative aspects characteristic of methods using different types of transplants;
— absence of foreign material;
— genioplasty is performed exclusively with local tissues;
— predictable result, the possibility of changing the position of the chin fragment of the lower jaw depending on the wishes of the patient and parents during the distraction process.
Children with congenital and acquired pathology of the lower jaw in 80% of cases need to eliminate underdevelopment and/or defects not only of the branch, but also of the body of the lower jaw. Existing two-stage methods significantly increase treatment time.
Advantages of the method of simultaneous elimination of underdevelopment of the branch and body of the lower jaw:
— acceptable appearance of the patient;
— there are no additional postoperative scars on the skin from the rods;
— unlimited retention period;
— the risk of developing inflammatory processes is significantly reduced;
— easier care of the KDA.
Bony KDA for the midface has the following advantages:
— ensuring rigid fixation of bone fragments during periods of distraction and retention, which is one of the main conditions for the maturation of bone regenerate;
— the ability to perform compression of bone fragments after their osteotomy, which is the main prevention of postoperative bleeding;
— strictly dosed movement, i.e. the size of the regenerate always corresponded to the duration of distraction, for example, with distraction for 20 days at 1 mm per day, the length of the regenerate was 20 mm;
— device weight 5 g;
— acceptable appearance of the patient;
- normal oral hygiene;
— simple care of the distraction apparatus during distraction and retention;
— the retention period is not limited;
— the possibility of using CDA in early childhood;
— it is possible to change the position of the middle zone of the face depending on the wishes of the patient and parents during the process of distraction.
Thus, the use of CDO currently makes it possible to significantly increase the effectiveness of treatment of children with complex maxillofacial pathologies of a congenital and acquired nature, and also makes it possible to provide real medical care to children with deformities and defects of the facial skull using a gentle method.
The CDO method is a priority in pediatric practice, and its further development and implementation allows us to consider it the main one in the treatment of children with defects and deformities of the maxillofacial and craniofacial areas.
Widespread implementation of the distraction method will significantly increase the efficiency and effectiveness of reconstructive surgical interventions, reduce the time of rehabilitation and patients’ stay in a hospital bed. To a large extent, there will be no need to use endoprostheses and highly traumatic methods for eliminating defects. There is no need to solve complex problems of eliminating secondary deformities in adult patients, since children will enter “adult” life having undergone comprehensive rehabilitation.
Authors:
prof. V.V. Roginsky
Doctor of Medical Sciences D.Yu. Komelyagin
Candidate of Medical Sciences S.A. Dubin