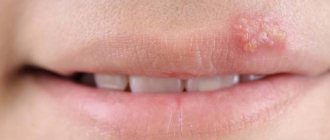
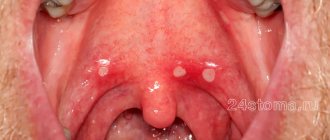
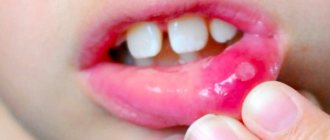
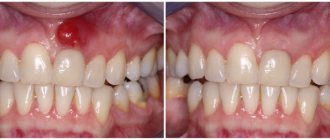
Bacterial stomatitis: before and after photos
The causes of infection may be:
- pockets of bacteria accumulation on carious teeth;
- germs entering the mouth due to herpes;
- infection during treatment - bacterial stomatitis can develop if the doctor does not comply with antiseptic rules;
- chronic diseases of various organs;
- contact with a sick person (for example, a kiss).
Symptoms of infectious stomatitis are, first of all, redness of the oral mucosa in the place where microbes entered the wound, swelling, and in the necrotic form, a rash. In children, cracks may form in the mucous membrane, and the gums begin to bleed. The damaged area is itchy and painful.
If bacterial stomatitis is not treated, the temperature rises, a headache appears, the lymph nodes and tonsils become inflamed, and due to intoxication of the body, the rash spreads throughout the body. Children may develop a sore throat and experience pain in the knee joints.
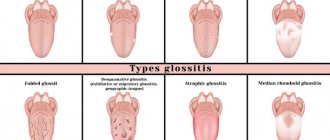
Types of stomatitis
The treatment regimen for stomatitis in children is based on the type of disease. There are several types of stomatitis:
- bacterial;
- viral, including herpes;
- fungal;
- aphthous;
- angular;
- allergic;
- traumatic.
All types of stomatitis occur in children, but the most common among children under 3 years of age are aphthous, candidal, herpetic and allergic. An increase in the incidence of traumatic stomatitis is usually associated with a period of active growth of primary teeth.
It is important to understand that in some cases, stomatitis is combined with other diseases with similar symptoms and is the first sign of more serious diseases. For example, with cheilitis - inflammation of the mucous membrane and red border of the lips, food allergies, etc.
Treatment of bacterial stomatitis
Self-medication for infectious stomatitis is completely excluded, since it is necessary to accurately identify the pathogen and select drugs that suppress it. Such studies are carried out in the laboratory. This is especially important when it comes to babies. To prevent possible complications, parents of a baby should immediately consult a doctor as soon as they see an inflamed scratch or swelling in the child’s mouth.
When treating bacterial stomatitis, the following are used:
If necrosis has developed, dead tissue is removed surgically, after which it is necessary to completely sanitize the oral cavity.
In parallel with medical measures to eliminate the symptoms of bacterial stomatitis, the patient is prescribed a diet. During this period, it is necessary to ensure maximum sparing of the oral mucosa, limit the consumption of carbohydrates and enrich the diet with vitamins and proteins.
- Superficial (catarrhal). In this case, symptoms of intoxication manifest themselves in a deterioration in appetite and an increase in temperature. There is discomfort when chewing and swallowing food, and the secretion of saliva periodically increases. When examining the oral cavity, a white coating on the tongue is found (on its lateral surfaces there are clearly visible imprints of teeth), bleeding gums, and hyperemia of the mucous membrane. Lack of treatment for catarrhal bacterial stomatitis leads to the disease progressing to the next, more severe form.
- Deep (ulcerative-necrotic). The patient's condition worsens. Symptoms of intoxication intensify: a person has a headache, the temperature rises to high levels, sleep and appetite are disturbed, weakness, irritability, and lethargy appear. Also, bacterial stomatitis in this form is characterized by pain when chewing, bad breath, and increased salivation. When examining the oral cavity, bleeding gums, hyperemia of the mucous membranes, and the presence of ulcers are revealed - first small, covered with a grayish coating, then enlarged, deep, with traces of tissue decay. Immunostimulants. They are necessary to boost immunity and prevent new outbreaks of the disease. These drugs have local and general effects. The doctor selects the optimal treatment option depending on the patient’s condition. For the same purpose, it is recommended to take a course of vitamins.
- Antibiotics. They are prescribed when bacterial stomatitis has become severe or the cause of the disease is systemic diseases of the internal organs. Effective remedies that stop infection directly in the oral cavity are ointments that contain an antibiotic. They give excellent results if the causative agent is a coccal infection. Among the drugs for oral administration in the treatment of bacterial stomatitis, penicillin, lincomycin, gentamicin, kanacimin and others are used.
- Antiseptics. At the initial stage and in the middle of the disease, rinsing with a chlorhexidine solution and treating the mucous membranes of the oral cavity with an anti-inflammatory gel with an analgesic effect are recommended. After the disappearance of acute symptoms, treatment of bacterial stomatitis continues with the help of epithelializing agents that promote rapid healing of defects.
Features of treatment
As is often the case with diseases that are at the intersection of several areas of medicine, inflammatory lesions of the oral mucosa are one of the least studied areas of dentistry. Therefore, several specialists can be involved in the treatment of stomatitis in children in the mouth: pediatrician, dentist, dermatologist, immunologist-allergist, otolaryngologist, etc. This is especially convenient when you go to a multidisciplinary clinic.
Self-medication of stomatitis is unacceptable, and although it is now easy to find ready-made treatment regimens and folk recipes, it is important not to experiment with the baby’s health.
Conservative treatment is mainly used, which involves treating the underlying cause of the disease. Your doctor may prescribe the following medications:
- antibacterial drugs (systemic and local in the form of ointments): for bacterial inflammation;
- antiviral agents for herpes and other types of viral stomatitis;
- antifungal drugs for fungal diseases;
- antihistamines - both for allergic origin of stomatitis, and as part of complex therapy to reduce swelling and itching;
- symptomatic drugs - anti-inflammatory, analgesic, antipyretic.
Treatment of candidal stomatitis in infants should be carried out with caution. At the same time, it is important to pay attention to your health; sometimes the cause of such a disease can be insufficient breast hygiene during lactation.
Often, only local remedies are sufficient, but make sure that the entire oral cavity is treated with the rinse - inflammatory agents can be found on the entire surface of the mucous membranes. Healing applications can be used to a limited extent, only on areas of inflammation.
Treatment of stomatitis of any kind in children involves strict adherence to a diet. The diet should be gentle, it is important to avoid salty, spicy, sour foods and drinks, serve the child warm meals, and limit the consumption of sweets.
If traumatic stomatitis occurs, the doctor will prescribe medications to speed up healing. However, it is very important to prevent re-injury. If it was caused by sharp edges of a tooth or filling, this cause should be eliminated. The doctor will suggest grinding off the filling or replacing it, and will also choose the appropriate option for restoring the shape of the crown in case of chips and cracks.
Prevention of stomatitis
You can reduce the risk of developing stomatitis using the following recommendations:
- regular washing of toys, bottles, pacifiers, breast hygiene if the baby is breastfed;
- general strengthening activities: walks, wet cleaning, a balanced diet, moderate hardening, adherence to a daily routine;
- fighting bad habits of biting nails, pencils, etc.;
- regular dental examinations and timely interventions in case of dental injuries.
The dentists of the Family Doctor clinic treat and prevent stomatitis in children.
Advanced equipment allows us to quickly and accurately assess the condition of the oral cavity and perform the necessary studies in a short time. We practice modern approaches to the treatment of inflammatory diseases of the oral cavity and adhere to an individual approach to each small patient. Consultations with a pediatric dentist are available by appointment. To make an appointment, call the single contact center or fill out a special online appointment form with a pediatric dentist on the website, or you can also visit the clinic’s reception in person.
What is aphthous stomatitis
The exact mechanisms of development of aphthous stomatitis are still unknown.
It is generally accepted that with aphthous stomatitis, the infection enters the oral cavity, but does not cause a protective reaction in the body's immune cells. They simply do not recognize the pathogen. The infection changes the composition of saliva, this causes the activity of lymphocytes and the immune system attacks areas of the oral mucosa as a foreign chemical agent.
As a result of this confrontation, erosions form on the mucous membrane.
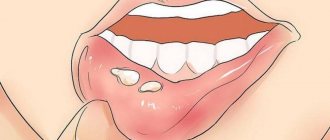
Aphthae have a round or oblong shape with a diameter of up to 5 mm. Outwardly, they resemble ulcers, covered with a white or gray coating and outlined with a red rim. On the mucous membrane, aphthae are located in groups or separately.
If more than three canker sores have formed in the mouth, this is a severe form of stomatitis. Despite their small size, the ulcers are painful and interfere with eating and talking. With stomatitis, the temperature may rise and weakness may appear.
If a person's immune system is weak, it will continue to interpret the presence of foreign chemicals in the mouth as a danger and canker sores will become chronic. Therefore, it is important to start treatment of aphthous stomatitis on time and carry it out under the supervision of a doctor.
Reasons for development
Stomatitis often occurs in people with reduced immunity and impaired microflora. If these 2 conditions are observed simultaneously, then even opportunistic microorganisms can cause severe inflammatory processes. Many other factors also influence the development of the disease.
Inflammation of the oral mucosa can occur in the following cases:
- mechanical, chemical, thermal injuries - hot burn, injury from solid food, cheek bite, etc. leads to tissue damage, penetration and spread of infection;
- poor nutrition, lack of vitamins, especially C, group B, minerals - zinc, iron and others;
- failure to comply with hygiene rules, eating unwashed fresh berries, vegetables, fruits, dirty hands while eating;
- treatment with medications that reduce salivation, antibiotics that destroy beneficial microflora, and a number of other medications;
- Frequent brushing of teeth with a paste containing sodium lauryl sulfate leads to a decrease in saliva secretion and dry mucous membranes, which become more susceptible to aggressive substances;
- poor-quality prosthetics and dental treatment due to which the gums are constantly injured;
- smoking, drinking alcohol;
- dehydration with prolonged diarrhea, vomiting.
Stomatitis often occurs during pregnancy due to hormonal imbalance. At risk are patients with diseases of the heart, blood vessels, gastrointestinal tract, pathologies of the immune and endocrine systems, and those with helminthic infestation. In diabetes mellitus, the aphthous form is diagnosed. People who use hormone inhalers to relieve asthma attacks suffer from candidiasis.
To answer the question whether stomatitis is contagious or not, differential diagnosis is necessary. Bacteria, viruses, and Candida fungi can be transmitted from person to person. The most contagious is the viral form of the pathology. However, with good immunity, the infection will not necessarily develop. It is also important how stomatitis is transmitted. If this is direct contact, for example a kiss, then the risk of getting sick is higher.
Causes of aphthous stomatitis
Aphthous stomatitis can be an independent disease or develop as a result of complex causes. Among them:
- Using aggressive agents that dry out the oral cavity (for example, sodium lauryl sulfate) during daily oral hygiene. The mucous membrane becomes more vulnerable, especially to sour and pungent tastes, and ulcers easily form on it.
- Mechanical damage to the oral cavity. Accidental biting of the inner surface, scratches from fillings and dentures, sharp chips of a tooth, rough traumatic food violate the integrity of the mucous membrane, and the resulting ulcer can serve as the beginning of the disease.
- Nervous tension and stress.
- Unbalanced nutrition, diets, nutrient and mineral deficiencies. Particularly critical is the lack of iron, zinc, folic acid, selenium, and vitamins B and C.
- Allergy to food. Products with gluten (flour), apples, tomatoes, chocolate, seafood and some food additives are critical.
- Menstrual cycle in women. Codependency with aphthous stomatitis is observed in only 10–15% of cases.
- Genetic predisposition.
- Chronic blood diseases, gastrointestinal tract, immunodeficiencies.
- Long courses of taking nonsteroidal drugs, medications for arrhythmia and high blood pressure.