From this article you will learn:
- how to treat aphthous stomatitis in children,
- symptoms and treatment of aphthous stomatitis in adults,
- list of effective drugs.
The article was written by a dentist with more than 19 years of experience.
Aphthous stomatitis is a disease in which one or more round ulcerations appear on the oral mucosa, which are covered with a necrotic coating of a gray or yellowish tint. Such ulcers (synonymous with aphthae) are not the result of acute infections, and therefore are not contagious, but nevertheless, such damage to the mucous membrane will require specific therapy.
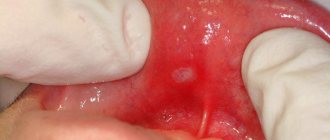
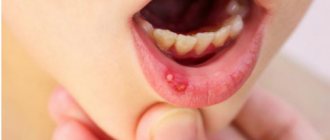
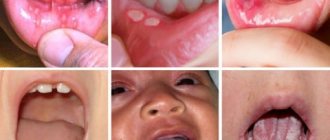
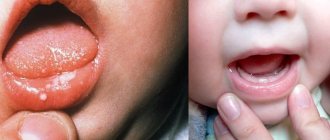
According to statistics, up to 20% of the population suffers from this form of stomatitis. Young children, as well as adults aged 20 to 30 years, are especially susceptible to this disease. In people of more mature age, there is a dependence: the higher the age, the less likely it is to develop. Aphthous stomatitis has a code according to ICD 10 - K12.0. Below you can see what this disease looks like in children and adults.
Aphthous stomatitis in children: photo
Aphthous stomatitis: photos in adults
The most important thing in treating stomatitis is to first correctly determine its form. Indeed, depending on its form, and it can be either herpetic or aphthous stomatitis, treatment for both adults and children will be completely different. Therefore, if you are not very sure of the diagnosis, it is best to familiarize yourself with the symptoms of both forms before starting treatment.
Types of disease
According to ICD-10, aphthous stomatitis is assigned code K.12. Within the code there are three qualifying diagnoses, including K.12.0 - “recurrent aphthae of the oral cavity,” which also includes aphthous ulcers.
According to the form of occurrence, acute and chronic aphthous stomatitis are distinguished. The first is characterized by the appearance of ulcers and severe hyperemia - swelling, redness of the mucous membranes. Severe pain occurs, especially when eating or talking. Submandibular lymph nodes may enlarge and body temperature may rise.
Chronic recurrent aphthous stomatitis may be the result of improper or untimely treatment, as well as the inability of the immune system to cope with the disease. It is characterized by periodic exacerbations. Outside of exacerbation, symptoms may be erased or completely absent.
The disease is classified into three forms depending on the severity:
- light. From 1 to 2 afts up to 10 mm in size. Moderate pain during mechanical action, relapses occur no more than 2 times a year;
- average. Up to 5 aft, the course of treatment takes up to 3 weeks. The pain is quite pronounced, there is an enlargement of the lymph nodes, relapses up to 2 times a year;
- heavy. Multiple aphthae appear, severe pain. An increase in temperature occurs, and symptoms of general intoxication appear. Treatment takes up to a month, relapses occur up to 6 times a year.
Also, according to the form of occurrence, the following types of inflammatory diseases are distinguished:
- fibrous: blood microcirculation in the upper layer of the mucosa is disrupted, aphthae appear, covered with a fibrous film (plaque). Such ulcers heal completely within 14 days. The disease affects the mucous membrane of the lips, the lateral surfaces of the tongue, and transitional folds. This stomatitis recurs up to 3 times a year;
- necrotic. The epithelium is destroyed, the mucosal area dies. Replacement of tissues with normal epithelium takes from 14 to 30 days. This aphthous stomatitis is not accompanied by acute pain; it is usually observed in patients with severe diseases, including blood pathologies;
- grandular. Damage to the ducts of the minor salivary glands occurs. In this regard, aphthae form close to the glands, and drying of the mucous membranes of the oral cavity occurs due to a decrease in saliva production. Ulcerations are painful and heal within 1–3 weeks;
- scarring. Damage to the cavity of the salivary glands leads to the involvement of connective tissue in inflammation. Aphthae are observed both at the location of the glands and on the mucous membranes of the pharynx and palate. The disease develops into large painful ulcers (up to 1.5 cm). Healing takes up to 12 weeks; after the acute process, pronounced scars remain;
- deforming. The most severe form of the disease, which provokes changes in connective tissue. Aphthae heal extremely slowly, which is accompanied by deformation of the palate, lips, and sometimes narrowing of the oral cavity occurs (if aphthae was observed in the corners of the mouth).
Ask a Question
Symptoms
The disease has rather sparse symptoms. Visually, it is easy to identify by the presence of characteristic ulcers on the inside of the lips, cheeks, soft palate and tongue (rarely). Keratinized (fixed) gums are not affected by aphthous stomatitis, which is another difference between aphthous stomatitis and herpetic stomatitis. At the initial stage of aphthae, the patient usually feels discomfort and burning, and the temperature may rise slightly. Diagnosis involves a visual examination, as well as taking blood tests and mucosal smears if the doctor suspects the presence of concomitant diseases.
Causes of aphthous stomatitis
Not all causes of aphthous stomatitis are fully understood. The mechanism of aft formation is often associated with activation of the local immune system - immune cells begin to destroy the epithelium of the mucous membranes, which leads to ulcers.
Local reasons include the following:
- allergic reactions;
- pathogenic microorganisms;
- mechanical damage (biting mucous membranes, injury from sharp edges of fillings or orthopedic, orthodontic structures);
- temperature or chemical influences.
Systemic causes of aphthous stomatitis:
- menstruation, pregnancy in women;
- sudden cessation of smoking;
- enteropathy, celiac disease, malabsorption;
- blood diseases;
- diseases of the immune system;
- lack of vitamins;
- other systemic diseases (lupus erythematosus, Crohn's disease, HIV infection, etc.).
Conclusions:
Aphthae in the mouth recur at some point in life in almost 20% of all people, most often in the second decade of life.
It is difficult to establish a clear and unambiguous reason.
If recurrent aphthae occurs, the pediatrician, physician, or dentist should consider the possibility that rare aphthae are a manifestation of a serious systemic disease.
In such situations, the gastroenterologist must exclude celiac disease, Crohn's disease and ulcerative colitis.
4, total, today
Symptoms of aphthous stomatitis
Usually, 1–2 days before the appearance of aphthae, areas of the mucous membrane with increased sensitivity are detected, and a burning sensation may occur. The aphthae themselves are round, have clear boundaries, and are covered with a gray or yellowish coating. Their size, as a rule, does not exceed 1 cm, and the mucous membranes around them turn red.
Such areas of erosion heal within up to 2 weeks without scarring. But in 1 case out of 10, the diameter of the ulcers is more than 1 cm, they affect deeper areas of tissue, and the borders of the pathological area may look raised. Healing in this case takes up to 6 weeks, after which a scar forms.
Aphthous stomatitis is characterized by damage to the mucous membranes of the cheeks, the inside of the lips, the soft palate, tonsils, and the lateral surfaces of the tongue. This is due to the lack of keratinization of the epithelium in these areas. Much less often, aphthae appear on the hard palate, back of the tongue, and gums.
Diagnostic features
At the initial appointment, the dentist examines the oral cavity and analyzes complaints. To make an accurate diagnosis, you need to distinguish this form of the disease from others, as well as differentiate it from other pathologies that have similar symptoms. For extensive lesions, different diagnostic methods may be used:
- clinical blood tests;
- microflora smear;
- blood for PCR to determine the causative agent of the disease;
- biopsy (if indicated).
They are also necessary for recurrent forms of the disease. In simple cases, laboratory diagnostics are not required; aphthae are determined visually by an experienced specialist.
With the help of a comprehensive examination, the doctor will determine which microorganism caused inflammation with subsequent ulceration of the mucous membrane. He also differentiates the disease from herpetic stomatitis and oncological pathology.
Features of treatment
The main goal of treating aphthous stomatitis is to completely get rid of the disease or at least reduce the frequency of relapses to a minimum. Therapy is aimed at relieving inflammation, relieving unpleasant symptoms, and accelerating the recovery processes of the mucous membrane.
For each specific case, the doctor will develop a set of measures. The main ones include local and systemic drug treatment.
Rinsing with antiseptics can be done using medications or mouth rinses that contain antibacterial components. An alternative to rinsing is to use a spray. Typically, the treatment regimen includes 2-3 sessions of 1-minute rinsing immediately after brushing your teeth.
Local treatment methods include the application of gels with anti-inflammatory and analgesic effects.
Occlusive agents can reduce pain and speed up the healing of mucous membranes. They form an insoluble film on the ulcer, protecting the affected area from exposure to adverse factors.
Local glucocorticoid therapy is used against the background of immune diseases, as well as when standard measures are ineffective. They eliminate pain and quickly relieve inflammation, shortening the healing period. Such products are used only according to indications and are available with a prescription. In some cases, it is advisable to inject the drug under the base of the ulcer; this is done by a doctor.
Epithelialization drugs are used after acute inflammation has resolved. The specialist will prescribe a gel with an analgesic and healing effect, usually this occurs 5–6 days after the start of complex therapy.
Local laser therapy can relieve pain, speed up the healing process, and minimize the risk of relapse.
Systemic treatment of aphthous stomatitis in adults involves taking the following drugs:
- antihistamines (anti-allergic, anti-edematous effect);
- glucocorticoids (anti-inflammatory, analgesic effect);
- immunomodulators (to stimulate defenses and accelerate recovery).
And if antiallergic drugs can be recommended to any patient even in the absence of information about the exact causes of stomatitis, then other drugs are prescribed only according to indications: in case of acute severe course of the disease, frequent relapses, and the presence of severe systemic pathologies. An additional method of treatment is vitamin therapy - taking vitamins C, group B.
In addition to the main course of treatment, all patients without exception are recommended to adhere to a hypoallergenic diet, avoid taking too hot drinks and dishes, and spicy, irritating foods. It is better to give preference to toothpaste without sodium lauryl sulfate, this component can provoke the disease.
It is important to continue your oral hygiene, even if it is difficult. To make brushing your teeth easier, choose a soft toothbrush. If the disease recurs frequently, it is necessary to pay attention to the general state of health, promptly treat teeth and gums, replace fillings and dental structures.
Forecast and prevention of the disease
If you consult a doctor in a timely manner, the treatment prognosis is favorable. Strict adherence to the doctor’s recommendations allows you to achieve remission.
The main prevention of stomatitis is maintaining oral hygiene. In order not to injure the mucous membrane, it is recommended not to use a hard brush. From time to time it is worth using pastes with an anti-inflammatory effect (contain oak bark).
After each meal you need to rinse your mouth with an herbal solution or special compositions. Regular visits to the dentist twice a year increases the chance of noticing the first manifestations of the disease.
It is the responsibility of parents to ensure that the child washes his hands frequently and thoroughly with soap and rinses vegetables and fruits before eating them.
Features of treatment in children
The dentist will tell you how to treat aphthous stomatitis in a child. You can contact him at the direction of your pediatrician or on your own if you find characteristic ulcers in the oral cavity. The treatment regimen is the same as that used in the treatment of adult patients, but there are some differences: children under a certain age cannot rinse the mouth, so preference is given to drugs for application to mucosal ulcers. Otherwise, the treatment regimen is developed individually, taking into account the severity, symptoms of the disease, frequency of relapses, and the presence or absence of concomitant ailments in the child. Symptomatic therapy can be used to quickly alleviate the baby’s condition.
Specialists at STOMA clinics successfully treat aphthous stomatitis. By contacting us, you will receive qualified assistance, detailed recommendations on the treatment and prevention of relapse of the disease, and comprehensive assistance from dentists of all specializations, if necessary.