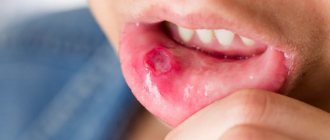
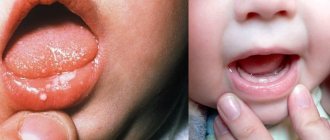
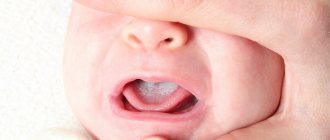
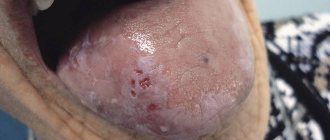
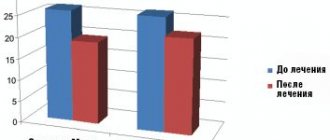
Stomatitis
This is a group of diseases characterized by inflammation of the oral mucosa with hyperemia, swelling, and an increase in the amount of mucus in the oral cavity.
Depending on the severity and depth of the lesion, even ulcers or foci of necrosis may form in the oral cavity, sharply disrupting the general condition - fever, weakness, anxiety, refusal to eat. There are many causes of the disease: mechanical, chemical, thermal, bacterial factors. Often the cause of the disease in infancy is contaminated nipples, toys and other objects that fall into the child’s mouth. Stomatitis often develops as a result of infectious diseases (measles, scarlet fever, influenza, whooping cough, etc.). The mucous membrane of the oral cavity acquires a bright red color, becomes swollen, and tooth marks are visible on the mucous membrane of the cheeks and tongue. Saliva becomes viscous and viscous. The mucous membrane is covered with a whitish coating. The tongue is dry, swollen, often with a brown tint, chewing is painful. The duration of the disease is from 1 to 3 weeks, the prognosis is favorable.
A general preventive rule for children and adults is to maintain good oral hygiene.
Thermal injuries of the oral mucosa in children.
They are rare in children, but are possible when eating hot food, especially milk and broth. The mucous membrane of the lips, the tip of the tongue, and the anterior part of the hard palate is mainly affected. It becomes swollen, hyperemic, and painful when touched. Less commonly, superficial intraepithelial vesicles form, which immediately burst. Upon examination in this case, fragments of white epithelium are visible on a hyperemic base. Prescribing antiseptics is unnecessary, since there is no deep defect in the epithelium, and therefore no conditions for secondary infection. For pain, painkillers are indicated: applications of a 0.5% solution of novocaine, lysozyme, 5–10% suspension of anesthesin in oil.
Gingivitis
An inflammatory process that causes swelling and tenderness of the soft tissues. If not treated in a timely manner, the problem worsens and becomes chronic.
The main causes of gingivitis:
- insufficient oral hygiene;
- thermal or chemical burns;
- use of certain medications;
- unbalanced diet (insufficient amount of vitamins in food)
- smoking;
- some infectious diseases;
- gastritis;
- ulcerative processes in the digestive system;
- caries.
Forms and types of gingivitis
Depending on the clinical situation and the nature of the development of the disease, acute and chronic gingivitis are distinguished. Acute gingivitis
manifests itself in the form of classic signs of the disease: redness, swelling and bleeding of the gums.
Chronic gingivitis
develops more quietly, without pronounced signs, but gradually leads to the growth of gum tissue (hyperplasia), which entails partial and complete coverage of the surface of the tooth crown by the gum.
Prevention measures
By following simple rules you can reduce the likelihood of serious oral diseases:
- Brushing your teeth at least 2 times a day after eating;
- Using dental floss and mouthwash;
- Balanced diet;
- Rejection of bad habits;
- Visit the dentist at least once every six months.
Stomach
Stomach
(lat.
ventriculus
) - a section of the digestive tract following the esophagus and preceding the duodenum. Upon examination, the position, size, and shape of the stomach depend on the position of the patient, the filling of the stomach, as well as on the condition of the surrounding organs - the liver, spleen, and intestines. The stomach, 5/6 of its size, lies to the left of the midline and only the pyloric part lies to the right.
The upper part of the stomach, being a continuation of the esophagus, is tightly fixed to the diaphragm by connective tissue cords. The entrance to the stomach (cardia) is located 3 cm from the place of attachment of the VII left costal cartilage to the sternum or at the level of the X-XI thoracic vertebra in the back. The highest point of the gastric vault lies on the fifth rib on the left along the parasternal line. The greater curvature, as the most mobile part of the stomach, is located more in front, adjacent, together with part of the anterior surface of the stomach, to the anterior abdominal wall. On the left, the upper part of the greater curvature touches the spleen, and the lower part touches the transverse colon.
The level of the lower edge of the greater curvature is very variable and depends on the type of constitution, gender, position of the patient (horizontal, vertical), the size of the abdomen, the tone and filling of the stomach. In women it is 1-2 cm lower than in men. In a horizontal position of the patient with an average filling of the stomach, it is located 2-3 cm above the navel in men, at the level of the navel in women, and when the stomach is full, the level drops lower. In the vertical position of the subject, the lower edge of the stomach in men is 3-4 cm, in women - 2-3 cm above the iliac line. The swollen and overcrowded transverse colon pushes the greater curvature from the anterior abdominal wall backward and upward. The outlet of the stomach is located at the level of the first lumbar vertebra, 1-2 cm to the right of the midline (Ionov A.Yu. et al.).
The normal residence time of the contents (digested food) in the stomach is about 1 hour.
Anatomy of the stomach
Anatomically, the stomach is divided into four parts:
- cardiac
(lat.
pars cardiaca
), adjacent to the esophagus; - pyloric
or pyloric (lat.
pars pylorica
), adjacent to the duodenum; - body of the stomach
(lat.
corpus ventriculi
), located between the cardiac and pyloric parts; - fundus of the stomach
(lat.
fundus ventriculi
), located above and to the left of the cardiac part.
In the pyloric section there is a pyloric cave
(lat.
antrum pyloricum
), synonyms
antrum
or
anturm
and
pyloric
(lat.
canalis pyloricus
).
The figure on the right shows: 1. Body of the stomach. 2. Fundus of the stomach. 3. Anterior wall of the stomach. 4. Greater curvature. 5. Small curvature. 6. Lower esophageal sphincter (cardia). 9. Pyloric sphincter. 10. Antrum. 11. Pyloric canal. 12. Corner cut. 13. A groove formed during digestion between the longitudinal folds of the mucosa along the lesser curvature. 14. Folds of the mucous membrane.
The following anatomical structures are also distinguished in the stomach:
- anterior wall of the stomach
(lat.
paries anterior
); - posterior wall of the stomach
(lat.
paries posterior
); - lesser curvature of the stomach
(lat.
curvatura ventriculi minor
); - greater curvature of the stomach
(lat.
curvatura ventriculi major
).
The stomach is separated from the esophagus by the lower esophageal sphincter and from the duodenum by the pyloric sphincter.
The shape of the stomach depends on the position of the body, the fullness of food, and the functional state of the person. With average filling, the length of the stomach is 14–30 cm, width 10–16 cm, length of the lesser curvature 10.5 cm, greater curvature 32–64 cm, wall thickness in the cardiac region 2–3 mm (up to 6 mm), in the antrum 3 –4 mm (up to 8 mm). The stomach capacity is from 1.5 to 2.5 liters (the male stomach is larger than the female). The normal weight of the stomach of a “conditional person” (with a body weight of 70 kg) is 150 g.
The stomach wall consists of four main layers (listed from the inner surface of the wall to the outer):
- mucous membrane covered with single-layer columnar epithelium
- submucosa
- muscle layer, consisting of three sublayers of smooth muscle:
- inner sublayer of oblique muscles
- middle sublayer of circular muscles
- outer sublayer of longitudinal muscles
Between the submucosal base and the muscular layer there is a nervous Meissner (synonym submucosal; lat. plexus submucosus
) plexus, which regulates the secretory function of epithelial cells, between the circular and longitudinal muscles - Auerbach (synonym intermuscular; lat.
plexus myentericus
) plexus.
Lectures for medical university students (video)
Lecture for students of the medical university “Ulcers of the stomach and duodenum” by Professor Yu.T. Tsukanova, in which he touches on the anatomy of the stomach and talks about its mucous membrane
Still from a video lecture by Dr. O.S. Tarasova “Physiology of Digestion” for students at the Faculty of Bioengineering and Bioinformatics of Moscow State University. M.V. Lomonosov
Frame “Stomach in children” from a video lecture by Ph.D. Gostishchevoy E.V. Anatomical and physiological features of the digestive organs in children. Methods and methods for studying the digestive system in children
Still from a video lecture by Lebedev A.V. Acid-dependent diseases of the gastrointestinal tract
Still from a video lecture by Abdiev G.Kh. Surgical diseases of the stomach and duodenum
Stomach mucosa
The mucous membrane of the stomach is formed by a single layer of columnar epithelium, a layer of its own and a muscular plate that forms folds (relief of the mucous membrane), gastric fields and gastric pits, where the excretory ducts of the gastric glands are localized.
In the proper layer of the mucous membrane there are tubular gastric glands, consisting of parietal cells that produce hydrochloric acid; main cells producing the proenzyme pepsin pepsinogen, and accessory (mucosal) cells secreting mucus. In addition, mucus is synthesized by mucous cells located in the layer of the surface (integumentary) epithelium of the stomach. The surface of the gastric mucosa is covered with a continuous thin layer of mucous gel consisting of glycoproteins, and underneath is a layer of bicarbonates adjacent to the superficial epithelium of the mucosa. Together they form the mucobicarbonate barrier of the stomach, which protects epithelial cells from the aggression of the acid-peptic factor (Y.S. Zimmerman). The mucus contains antimicrobial activity immunoglobulin A (IgA), lysozyme, lactoferrin and other components.
The surface of the mucous membrane of the body of the stomach has a pitted structure (see figure on the left, Matveeva L.V. et al.), which creates conditions for minimal contact of the epithelium with the aggressive intracavitary environment of the stomach, which is also facilitated by a thick layer of mucous gel. Therefore, the acidity on the surface of the epithelium is close to neutral. The mucous membrane of the body of the stomach is characterized by a relatively short path for the movement of hydrochloric acid from the parietal cells into the lumen of the stomach, since they are located mainly in the upper half of the glands, and the main cells are in the basal part. An important contribution to the mechanism of protecting the gastric mucosa from the aggression of gastric juice is made by the extremely rapid nature of gland secretion, caused by the work of the muscle fibers of the gastric mucosa. On the contrary, the mucous membrane of the antral region of the stomach (see the figure on the right) is characterized by a “villous” structure of the surface of the mucous membrane, which is formed by short villi or convoluted ridges 125–350 µm high (Lysikov Yu.A. et al.).
Still from video by Partsvania-Vinogradova E.V. The role of pH-metry in acid-related diseases
Stomach in children
In children, the shape of the stomach is not constant and depends on the constitution of the child’s body, age and diet.
In newborns, the stomach has a round shape; by the beginning of the first year it becomes oblong. By the age of 7–11, a child’s stomach does not differ in shape from an adult’s. In infants, the stomach is positioned horizontally, but as soon as the child begins to walk, it takes on a more vertical position. By the birth of a child, the fundus and cardiac part of the stomach are not sufficiently developed, and the pyloric part is much better, which explains frequent regurgitation. Regurgitation is also promoted by swallowing air during sucking (aerophagia), with improper feeding technique, short frenulum of the tongue, greedy sucking, and too rapid release of milk from the mother's breast.
| Age | Stomach volume, ml |
| newborns | 30–35 |
| 1 year | 250–350 |
| 2 years | 300–400 |
| 3 years | 400–500 |
| 8 years | 1000 |
Gastric juice
The main components of gastric juice are: hydrochloric acid secreted by parietal cells, proteolytic enzymes produced by chief cells and non-proteolytic enzymes, mucus and bicarbonates (secreted by accessory cells), intrinsic Castle factor (production of parietal cells).
The gastric juice of a healthy person is practically colorless, odorless and contains a small amount of mucus.
Basal secretion, not stimulated by food or otherwise, in men is: gastric juice 80-100 ml/h, hydrochloric acid - 2.5-5.0 mmol/h, pepsin - 20-35 mg/h. Women have 25–30% less. About 2 liters of gastric juice are produced in the stomach of an adult per day.
The gastric juice of an infant contains the same components as the gastric juice of an adult: rennet, hydrochloric acid, pepsin, lipase, but their content is reduced, especially in newborns, and increases gradually. Pepsin breaks down proteins into albumins and peptones. Lipase breaks down neutral fats into fatty acids and glycerol. Rennet (the most active enzyme in infants) curdles milk (Bokonbaeva S.D. et al.).
Stomach acidity
The main contribution to the total acidity of gastric juice is made by hydrochloric acid produced by the parietal cells of the fundic glands of the stomach, located mainly in the area of the fundus and body of the stomach.
The concentration of hydrochloric acid secreted by parietal cells is the same and equal to 160 mmol/l, but the acidity of the secreted gastric juice varies due to changes in the number of functioning parietal cells and neutralization of hydrochloric acid by alkaline components of gastric juice. Normal acidity in the lumen of the body of the stomach on an empty stomach is 1.5–2.0 pH. The acidity on the surface of the epithelial layer facing the lumen of the stomach is 1.5–2.0 pH. The acidity in the depths of the epithelial layer of the stomach is about 7.0 pH. Normal acidity in the antrum of the stomach is 1.3–7.4 pH.
On the graph: 24-hour pH-gram of the body of the stomach is normal (Storonova O.A., Trukhmanov A.S.)
Currently, the only reliable method for measuring gastric acidity is considered to be intragastric pH-metry, performed using special devices - acidogastrometers, equipped with pH probes with several pH sensors, which allows you to measure acidity simultaneously in different zones of the gastrointestinal tract.
Stomach acidity in relatively healthy people (who do not have any subjective gastroenterological sensations) changes cyclically during the day. Daily fluctuations in acidity are greater in the antrum than in the body of the stomach. The main reason for such changes in acidity is the longer duration of nocturnal duodenogastric reflux (DGR) compared to daytime, which throws duodenal contents into the stomach and, thereby, reduces the acidity in the lumen of the stomach (increases pH). The table below shows the average acidity values in the antrum and body of the stomach in apparently healthy patients (Kolesnikova I.Yu., 2009):
| Index | Day | Day | Night |
| Average acidity of the stomach body, units. pH | 3,2 | 3,1 | 3,3 |
| Average acidity of the antrum of the stomach, units. pH | 4,0 | 3,6 | 4,4 |
| Number of DGRs lasting more than 5 minutes | 29 | 12 | 18 |
| Number of DGRs reaching the body of the stomach | 11 | 5 | 6 |
The general acidity of gastric juice in children of the first year of life is 2.5–3 times lower than in adults. Free hydrochloric acid is determined during breastfeeding after 1–1.5 hours, and during artificial feeding – after 2.5–3 hours after feeding. The acidity of gastric juice is subject to significant fluctuations depending on the nature and diet, and the state of the gastrointestinal tract.
Gastric motility
In terms of motor activity, the stomach can be divided into two zones: proximal (upper) and distal (lower). There are no rhythmic contractions or peristalsis in the proximal zone. The tone of this zone depends on the fullness of the stomach. When food arrives, the tone of the muscular lining of the stomach decreases and the stomach reflexively relaxes.
| Motor activity of various parts of the stomach and duodenum (Gorban V.V. et al.) |
Gastric accommodation is a postprandial vagal reflex, leading to a decrease in the tone of the stomach (primarily in the proximal section) in response to food intake (see figure on the left). Gastric accommodation provides a reservoir for ingested food without a significant increase in intragastric pressure. Esophageal distension may also be accompanied by proximal gastric relaxation. So-called adaptive relaxation involves relaxation of the proximal stomach in response to stretching of the antrum. Adaptive relaxation ensures the creation of a pressure gradient inside the organ, which promotes mixing of food and its adequate grinding. Adaptive relaxation can be generated by both local (with the initiation of mechanoreceptors in the antrum) and vago-vagal reflexes.
| Application of electrodes to the patient's abdomen during electrogastrography |
In the proximal zone in the area of the greater curvature of the stomach, interstitial cells of Cajal are located, which form the rhythm of gastric contractions (on average 3 cycles per minute).
The resulting peristaltic waves are directed towards the duodenum. Their functional role is to push the contents of the stomach towards the pylorus. The motor function of the stomach is studied using electrogastrography. It is accepted that, depending on the frequency of the fundamental harmonic, the following occurs:
- normogastria (normal motility) - at a frequency of 2 to 4 cycles per minute
- bradygastria (reduced motility) - with a frequency of less than 2 cycles per minute
- tachygastria (increased motor skills) - at a frequency of 4 to 10 per minute.
The graph shows electrogastrograms of the stomach before (red curve) and after eating (green). The abscissa axis is seconds, the ordinate axis is millivolts (Popov A.I., Rudalev A.V.).
Using electroenterogastrography (which uses the same Gastroscan-GEM device, but the research methodology differs from electrogastrography), the following gastric motility disorders are detected:
- irritable stomach
- characterized by normal or reduced electrical activity of the stomach on an empty stomach with a subsequent increase in its electrical activity after eating by more than 1.5-2 times - lazy stomach
- characterized by normal electrical activity of the stomach on an empty stomach and a decrease in it after eating - asthenic stomach
- characterized by a high level of electrical activity of the stomach on an empty stomach and a decrease in it after eating (Rachkova N.S., Khavkin A.I.).
An important role in the implementation of the motor function of the stomach in children belongs to the activity of the pylorus, thanks to the reflex periodic opening and closing of which food masses pass in small portions from the stomach to the duodenum. In the first months of life, the motor function of the stomach is poorly expressed, peristalsis is sluggish, and the gas bubble is enlarged. In infants, there may be an increase in the tone of the stomach muscles in the pyloric region, the maximum manifestation of which is pyloric spasm. Cardiospasm sometimes occurs in older people.
Functional deficiency decreases with age, which is explained, firstly, by the gradual development of conditioned reflexes to food stimuli; secondly, the complication of the child’s diet; thirdly, the development of the cerebral cortex. By two years, the structural and physiological characteristics of the stomach correspond to those of an adult (Bokonbaeva S.D. et al.).
Stomach enzymes
Cells of the gastric mucosa secrete a large number of enzymes. The most important proteolytic enzymes of gastric juice: pepsin, gastrixin (pepsin C), and chymosin (rennin). The pepsin precursor (proenzyme) pepsinogen, as well as the proenzymes gastricsin and chymosin, are produced by the main cells of the gastric mucosa, and are subsequently activated by hydrochloric acid. Non-proteolytic enzymes of gastric juice are lysozyme, carbonic anhydrase, amylase, lipase and others.
Endocrine cells of the stomach
The gastric mucosa contains a large number of endocrine cells that produce a number of hormones.
35% of the endocrine cells of the stomach of a healthy person are enterochromaffin-like cells that secrete histamine, 26% are G-cells that secrete gastrin. In third place in number are D-cells that secrete somatostatin. The figure on the right shows a diagram of the fundic gland (Dubinskaya T.K.):
1 - mucus-bicarbonate layer 2 - surface epithelium 3 - mucous cells of the neck of the glands 4 - parietal cells 5 - endocrine cells 6 - chief (zymogenic) cells 7 - fundic gland 8 - gastric fossa
Microflora of the stomach
Until recently, it was believed that due to the bactericidal effect of gastric juice, microflora that penetrated the stomach died within 30 minutes. However, modern methods of microbiological research have proven that this is not the case. The amount of various mucosal microflora in the stomach of healthy people is 103–104/ml (3 lg CFU/g), including Helicobacter pylori
(5.3 lg CFU/g) detected in 44.4% of cases, 55.5% - streptococci (4 lg CFU/g), 61.1% - staphylococci (3.7 lg CFU/g), 50% - lactobacilli (3.2 lg CFU/g), 22.2% - fungi of the genus
Candida
(3.5 lg CFU/g).
In addition, bacteroides, corynebacteria, micrococci, etc. were sown in an amount of 2.7–3.7 lg CFU/g. It should be noted that Helicobacter pylori
was detected only in association with other bacteria.
The environment in the stomach turned out to be sterile in healthy people only in 10% of cases. Based on their origin, the microflora of the stomach is conventionally divided into oral-respiratory and fecal. In 2005, strains of lactobacilli that adapted (like Helicobacter pylori
) to existing in the sharply acidic environment of the stomach were discovered in the stomach of healthy people:
Lactobacillus gastricus, Lactobacillus antri, Lactobacillus kalixensis, Lactobacillus ultunensis
.
In various diseases (chronic gastritis, peptic ulcer, stomach cancer), the number and diversity of bacterial species colonizing the stomach increases significantly. In chronic gastritis, the largest amount of mucosal microflora is found in the antrum, in peptic ulcer disease - in the periulcerous zone (in the inflammatory ridge). Moreover, the dominant position is often occupied not by Helicobacter pylori
, but by streptococci, staphylococci, enterobacteria, micrococci, lactobacilli, and fungi of the genus
Candida
(Y.S. Zimmerman).
According to Engstrand L. (2012), in the stomach of a healthy person, in the absence of dominance of Helicobacter pylory
, the main volume of the gastric microbiota is represented by ten genera:
Prevotella, Streptococcus, Veillonella, Rothia, Haemophilus, Actinomyces, Fusobacterium, Neisseria, Porphyromonas
and
Gemella
, belonging to five types (lat.
phylum
) of bacteria:
Firmicutes, Proteobacteria, Bacteroidetes, Actinobacteria
and
Fusobacteria
.
Spectrum and frequency of occurrence of microorganisms in the mucous membranes of the esophagus, stomach and duodenum of healthy people (Julai G.S. et al.)
In addition to
Helicobacter pylori,
other representatives of the genus
Helicobacter
.
Patients in whom non-H. pylori Helicobacter species, suffered from gastritis, peptic ulcers, stomach cancer and MALT lymphoma. Although these bacteria are often incorrectly called " Helicobacter heilmannii
", a number of similar but distinct important bacterial species are actually implicated in the development of gastric pathologies, including
Helicobacter bizzozeronii, Helicobacter felis, Helicobacter heilmannii, Helicobacter salomonis
and
Helicobacter suis species.
Diagnosis of infections caused by non-H. pylori Helicobacter pylori agents is not always simple, partly due to their focal colonization in the human stomach (Starostin B.D. Treatment of Helicobacter pylori infection - Maastricht V / Florence consensus report).
Some diseases and conditions of the stomach
Some stomach diseases and syndromes (see):
- gastritis
Perforation of the stomach - a complication of peptic ulcer - acute gastritis
- chronic gastritis
- atrophic gastritis
- anacid gastritis
- superficial gastritis
- antral gastritis
- reflux gastritis
- Ménétrier's disease
- infectious gastritis*
- Helicobacter pylori
-induced gastritis - bacterial gastritis not associated with Helicobacter pylori
- Helicobacter heilmannii
- associated gastritis - enterococcal gastritis
- anisacidosis of the stomach
- strongyloidiasis of the stomach
- cryptosporidosis of the stomach
| Filippova M.P. Peptic ulcer disease. Lecture for the 2nd year of the FKP MGMSU named after. A.I. Evdokimova (video) |
- postprandial distress syndrome
*Classification of infectious gastritis follows the Kyoto global consensus.
Neoplasms:
- stomach cancer
- stomach polyps and polyp-like formations
- gastric adenomas
- Peutz-Jeghers syndrome
Gastric motility disorders:
- "irritable" stomach
- "lazy" stomach
Some symptoms that may be associated with stomach problems:
- stomach ache
- nausea
- vomit
- gastralgia
Acidity chart for duodenogastric reflux (Storonova O.A., Trukhmanov A.S.)
Patient Materials
- Vasilenko V.V. Stomach // www.gastroscan.ru. 2022.
- Agapkin S.N. The most important thing about the stomach and intestines. Peptic ulcer // Eksmo Publishing House LLC. Moscow. 2022. 53 p.
- Vasilenko V.V. Stomach and resorts / www.gastroscan.ru. 2018
The GastroScan.ru website contains: a subsection “Doctors' Advice” in the “Patients” section of the site, a subsection “Popular Gastroenterology” in the “Literature” section, as well as a subsection “Popular Gastroenterology” in the “Video” section, containing materials for patients on various aspects of gastroenterology.
Publications for healthcare professionals regarding gastric anatomy, physiology and diseases
- Matveeva L.V., Usanova A.A., Mosina L.M. Physiology of the stomach: monograph / Saransk, 2012. – 100 p.
- Butov M.A., Kuznetsov P.S. Examination of patients with diseases of the digestive system. Part 1. Examination of patients with stomach diseases. A textbook on propaedeutics of internal diseases for 3rd year students of the Faculty of Medicine. - Ryazan. — 2007.
- Rapoport S.I., Lakshin A.A., Rakitin B.V., Trifonov M.M. pH-metry of the esophagus and stomach in diseases of the upper digestive tract / Ed. Academician of the Russian Academy of Medical Sciences F.I. Komarova. — M.: ID MEDPRACTIKA-M. — 2005. – p. 208.
- Stupin V.A., Siluyanov S.V. Violation of the secretory function of the stomach in peptic ulcer // Russian Journal of Gastroenterology, Hepatology, Coloproctology. - 1997. - No. 4. - p. 23–28.
- Korotko G.F. Organization of gastric digestion // Bulletin of surgical gastroenterology. - 2006. - No. 1. - p. 17–25.
- Zimmerman Ya.S. Modern methods for studying the functions of the stomach and their diagnostic capabilities // RZHGGK. - 2011. - T.21. - No. 5. — P.4-16.
- Lysikov Yu.A., Goryacheva O.A., Tsvetkova L.N., Krasavin A.V., Gureev A.N., Tsvetkov P.M. Clinical and morphological features of duodenal ulcer in children // Pediatrics. 2011. Volume 90. No. 2. pp. 38–42.
- Levit R.M. Clinical, endoscopic and morphological characteristics of chronic gastroduodenitis in childhood. Abstract of dissertation. Doctor of Medical Sciences, 01/14/08 – pediatrics, YSMU, Moscow, 2016.
- Kolesnikova I.Yu., Volkov V.S. Diagnosis and treatment of acid-related diseases of the digestive tract. Guide for doctors / M.: Publishing House “Medical Information Agency”, 2014. - 432 p.
- Guseinov A.Z., Bronshtein P.G., Sazhin V.P. Stomach surgery monograph // St. Petersburg - Tula: Tula State University Publishing House, 2014. - 264 p.
On the website GastroScan.ru in the “Literature” section there is a subsection “Diseases of the stomach and duodenum”, containing publications for healthcare professionals. Back to section
Periodontitis
Periodontitis is an inflammation of periodontal tissues, which includes the teeth, ligaments, cementum and gums. Periodontitis as a disease is a consequence of gingivitis - a minor inflammation of the gums, the main cause of which is neglect of oral hygiene. If with gingivitis the inflammation spreads exclusively to the soft mucous membranes, then with periodontitis the ligaments that hold the teeth in the sockets are affected. This is why in 90% of cases when this disease is diagnosed, tooth mobility is observed, which eventually leads to their loss.
The most common causes of the disease are the following:
1. Improper or irregular oral care
. Dental plaque, which is present on the surface of the teeth and in the spaces between teeth, is not as safe a substance as it might seem at first glance. Soft and easily removed at the beginning, it goes through certain cycles of “development”. The result is the mineralization of plaque and its transformation into hard tartar. This process in most cases is observed in those who do not pay due attention to daily oral care or use an incorrectly selected toothbrush, toothpaste and mouthwash.
2. Poor blood supply to the gums
. Periodontitis is one of the most common problems among smokers. Substances contained in tobacco smoke lead to a narrowing of the blood vessels in the oral mucosa and their fragility, which impairs the blood supply to the gum tissue and supporting apparatus of the teeth. A slowdown in blood circulation and, as a consequence, the development of periodontitis is also facilitated by a lack of chewing load caused by eating habits (for example, the predominance of soft foods in the diet).
3. Nutrient Deficiency
. The lack of fresh vegetables, fruits, herbs, a sufficient amount of fish, meat and dairy products in the diet quickly leads to a lack of essential substances in the gum tissue. If poor nutrition is a permanent habit, then over time the metabolic processes in the gums are disrupted, which creates the ground for inflammation and periodontitis. A deficiency of vitamins A, C and group B can lead to negative consequences.
Treatment of periodontitis
Professional teeth cleaning is an integral step in the treatment of periodontitis. This procedure removes physical obstacles (plaque and tartar) that prevent the gums from returning to their previous position and tightly covering the teeth.
Drug treatment - the use of antiseptics for topical use. This need is due to the high risk of spread of inflammation and infection to other tissues.
Surgery
At an advanced stage of periodontitis, when the inflammation has spread deep into the bone tissue, surgical intervention becomes necessary. Such manipulations include partial excision of the gums (gingivectomy), washing of periodontal pockets with medicinal solutions, removal of stones, and flap operations. In some cases, surgical treatment of periodontitis involves the implantation of bone tissue substitutes or the application of collagen or artificial membranes to restore the supporting apparatus of the tooth.
Compliance with oral care rules
Without regularly removing plaque and protecting the oral cavity from bacteria, it is impossible to achieve sustainable results in the treatment of periodontitis. Hygiene procedures twice a day with properly selected products, the use of dental floss and rinses will help make recovery faster.
Chemical injuries to the oral mucosa in children.
These injuries are observed mainly in children 1–3 years old due to accidental ingestion of solutions of acids and alkalis used in everyday life. In this case, combined burns of the mucous membrane of the mouth, pharynx, and esophagus develop. The severity of the lesion is determined by the concentration of the drug and the duration of its effect. The mucous membrane becomes sharply hyperemic, then necrosis appears within a period of several hours to a day, the deepest usually on the lower lip. Necrotic tissues become saturated with fibrinous exudate; a thick film is formed, which is slowly torn off on the 7th - 8th day and at a later date. In an uncomplicated course, under such a film, tissue scarring and epithelization of the defect occur in parallel.
Chemical burns can be caused by many medications used in dental treatment: phenol, formalin, antiformin, acids, alcohol, ether, etc., so the dentist should be especially careful when using them, taking into account the easy vulnerability of the mucous membrane in children and the often violent reaction of the body in response to its damage.
TREATMENT OF CHEMICAL INJURIES OF THE ORAL MUCOSA IN CHILDREN.
For chemical burns in the first minutes and hours, it should be aimed at neutralizing the chemical agent with 1 - 2% solutions of sodium bicarbonate for acid burns and 1% hydrochloric acid solution or 3% citric acid solution for alkali burns. Further treatment consists of preventing secondary infection of the lesion and pain relief. For burns of the pharynx and esophagus, the child should be hospitalized in the ENT department.
Periodontal disease
Dental periodontal disease is a serious disease in which the last stage of gum inflammation occurs. This is often the cause of the development of infectious diseases, gastritis, stomach ulcers or cirrhosis of the liver. Even more often, the patient’s teeth simply fall out, and he cannot lead his usual lifestyle or eat his favorite food.
How to recognize periodontal disease
The signs of this dental disease are unclear and blurred. The patient is most often concerned about:
- exposure of the necks of the teeth;
- presence of tartar;
- burning gums;
- discomfort when eating.
There are 3 stages of periodontal disease:
- Easy. The patient has no complaints; very rarely there is a reaction to cold or hot food. The presence of periodontal disease can be determined during a dental examination. The mild stage of the disease is best treated.
- Average. The roots of the teeth are exposed by an average of 4-6 mm. The patient begins to experience a burning sensation in the mouth, and there is an acute reaction to eating hot, cold or sour foods.
- Heavy. The roots of the teeth are exposed by 8-10 mm. Chewing food causes severe pain.
Treatment methods
Diagnostics
Before starting treatment for periodontal disease, the dentist conducts an initial examination, during which he determines the extent of damage to the teeth and gums: which teeth can be restored and which will have to be removed. This is necessary in order to draw up an algorithm for further actions. The patient is then sent to the diagnostic room to take targeted and panoramic X-rays. Using them, the periodontist determines the depth of the pockets and the condition of the bone tissue.
Removing plaque and tartar
Inflammation of the gums, which is always observed with periodontal disease, mainly occurs due to soft plaque, subgingival and supragingival calculus. The main reason for their appearance is poor oral hygiene. Therefore, the specialist’s task is not only to treat the disease, but also to teach the patient proper hygiene.
General and local therapy
To increase immunity, the patient is prescribed a complex of vitamins and anti-inflammatory drugs. If the inflammation is minor, the dentist will prescribe a course of local therapy, which can be done independently at home.
Splinting teeth
An increase in tooth mobility indicates that the jawbone and soft tissue around them have begun to rapidly deteriorate. To prevent the teeth from changing position and falling out (for example, they may fan out), they are held together with fiberglass tape and filling material. This is also necessary before surgical treatment.
Surgical operations
If periodontal pockets reach 5-10 mm, it is impossible to prevent the progression of the disease without surgical intervention. First, the pockets are cleaned of granulations and food deposits. This procedure is called curettage. It comes in two types - open and closed.
Closed is carried out with special instruments, curettes. It is carried out only for periodontal disease at the initial stage (pockets reach 3 mm), when there is slight inflammation of the gums.
Open curettage is necessary in advanced stages of periodontal disease. With its help, all granulations and food deposits are completely removed. This operation is more difficult to perform. To completely clean out the pockets, incisions are made in the gum. Flaps of the mucous membrane are peeled away from the bone and the root surface is cleaned with curettes and an ultrasonic scaler. To restore bone tissue, the periodontist implants synthetic bone.
Next, the patient undergoes flap surgery to prevent receding gums. The doctor removes a 1.5 mm marginal strip of gum, since after prolonged inflammation the gum changes in such a way that it can no longer adhere normally to the tooth. After this, the mucous membrane flaps are pulled to the neck of the tooth.
Timely diagnosis and choosing the right treatment will help stop periodontal disease and maintain healthy teeth!