Author of the article:
Soldatova Lyudmila Nikolaevna
Candidate of Medical Sciences, Professor of the Department of Clinical Dentistry of the St. Petersburg Medical and Social Institute, Chief Physician of the Alfa-Dent Dental Clinic, St. Petersburg
Candidiasis or, otherwise, thrush is an infectious disease, the main cause of which is infection with Candida fungi. These fungi belong to the same species as yeast and are part of the natural microflora of the vast majority of healthy people. The maximum concentration of these opportunistic microorganisms is observed in the intestines, nasopharynx, and vagina; Some fungi can also be found on the surface of the skin.
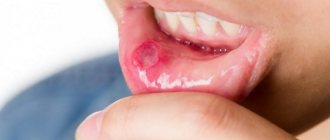
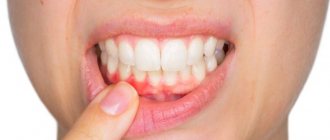
In a normal, healthy state of the body, the fungus does not cause any unpleasant symptoms. However, when the immune system is weakened and other provoking factors appear, Candida actively multiplies, resulting in discomfort, itching, burning and other manifestations of thrush. This disease can affect various tissues and organs; Candidiasis of the oral mucosa is also common.
Most often, infants suffer from this disease: according to statistics, up to 20 percent of children under the age of one year have suffered from candidiasis at least once. About 10 percent of people over 60 also suffer from symptoms of this infection. It occurs more often in women than in men; very often, signs of the disease appear in smokers. There are many other factors that contribute to the development of candidiasis in the mouth.
Causes of oral candidiasis
The main reason for the occurrence is a decrease in immune status, as a result of which the uncontrolled proliferation of microflora begins. Reduced immunity is observed in older people and infants, in patients suffering from HIV, AIDS and other diseases associated with immunodeficiency, in those who regularly expose the body to excessive stress, neglect the rules of a healthy diet and violate work and rest patterns. Risk factors include reasons such as:
- Use of medications.
Taking antibiotics, immunosuppressants (drugs that suppress the immune system) and some other medications leads to disruption of the immune system and the natural balance of microflora in the body. Oral contraceptives, which affect hormonal levels, have a similar effect. - Pregnancy.
During pregnancy, a sharp and significant change in hormonal levels occurs, which can lead to a surge in the activity of pathogenic and opportunistic microflora. - Radiation and chemotherapy.
Often occurs in patients undergoing drug and radiological treatment for cancer. - Injuries to mucous membranes.
Violation of the integrity of the mucous membranes leads to loss or deterioration of the barrier function, as a result of which the fungus enters deep into the tissues, causing inflammation and other symptoms. Small, but constantly recurring injuries are especially dangerous - for example, when wearing incorrectly fitted dentures or braces. - Overwork and stress.
Prolonged stress of physical and mental forces leads to a deterioration in the protective function of the body. Similar consequences are caused by hypothermia or overheating, regular lack of sleep, insufficient, excessive or simply unbalanced nutrition, abuse of alcohol, nicotine, and narcotic substances. - Hypo- and vitamin deficiency.
May be caused by a lack of nutrients, in particular vitamins B and C. - Somatic diseases.
Frequent companions of candidiasis include tuberculosis, dysbacteriosis and other pathologies of the gastrointestinal tract, diseases of the adrenal glands and other endocrine glands. Candidiasis is a contagious disease. A large number of pathogenic microorganisms are transmitted through kissing and sexual contact, through the use of shared dishes, towels and other household items. Infection can also occur during childbirth (vertical transmission from mother to fetus). In addition, there is a risk of infection through contact with infected pets.
Risk factors for development
The likelihood of infection increases with casual sexual intercourse, uncontrolled use of antibiotics and drugs that disrupt the natural microflora. Foods with large amounts of sugar and carbohydrates create a favorable environment for fungal growth. Excessive sweating also leads to an exacerbation of candidiasis, so it is necessary to wear cotton underwear that allows the skin to breathe and moisture to evaporate.
At the same time, excessive cleanliness can also cause harm. We are talking about douching. It should not be used as a method of contraception, since it is not effective, and also as a means of hygiene, because it leads to the leaching of the protective flora. If you experience discomfort, you should first consult a doctor.
Types of disease
The clinical picture of oral candidiasis is classified:
- For clinical and morphological.
- With the flow.
- By localization.
Clinical and morphological is divided into:
- Hyperplastic.
- Erosive-ulcerative.
- Pseudomembranous.
- Atrophic.
The clinical picture, classified according to the course, is divided into:
- Chronic.
- Spicy.
By localization:
- Cheilitis.
- Gingivitis.
- Glossitis.
- Stomatitis.
- Tonsillitis, etc.
Based on the clinical picture, oral candidiasis comes in several types:
- Chronic hyperplastic.
- Candida infection.
- Chronic atrophic.
- Acute pseudomembranous.
- Chronic pseudomembranous.
- Acute atrophic.
Diet for fungus in the mouth
Antifungal Diet
- Efficacy: no data
- Terms: 3-6 months
- Cost of products: 1500-1600 rubles. in Week
In addition to complex antifungal treatment, patients are strongly recommended to follow a strict diet consisting of foods without vinegar, sugar, yeast and alcohol. in vitamins and strengthening the immune system is also recommended The menu should include bananas, onions, garlic, asparagus, chicory, olive oil, seafood, legumes, and buckwheat.
Symptoms
Infection of the oral mucosa by Candida fungus can take various forms, each of which has its own characteristics of symptoms. The most common forms of the disease are candidal angulitis, glossitis, cheilitis, and stomatitis. There are both acute and chronic forms of the disease.
- Pseudomembranous acute candidiasis is the most common form and most often occurs in infants and the elderly. This form is characterized by the appearance of severe swelling and hyperemia (redness) of the mucous membranes. In addition, a characteristic whitish coating forms on the surface of the lips, palate, back of the tongue and the inside of the cheeks. If the plaque is scraped off, the surface of the mucous membrane underneath will be macerated (softened) or ulcerated and bleeding. In this case, patients complain of pain, burning or itching in the mouth; Eating becomes very difficult. Very often the process spreads to the esophagus and pharynx.
- Acute atrophic candidiasis of the oral mucosa usually develops due to the lack of adequate treatment. The upper part of the mucous membranes (epithelium) is exfoliated, the mucous membrane becomes thin, red or, on the contrary, swollen. The patient’s tongue and the corners of the lips also acquire a bright red color; the papillae on the tongue atrophy and smooth out. The plaque is absent or is found only in hard-to-reach places.
- Hyperplastic chronic candidiasis is characterized by the formation of a large number of papules and plaques of irregular or round shape. They are located close to each other on the mucous membrane of the tongue and cheeks and often become soldered and fused. Around each such formation there is a thin rim of reddened, inflamed tissue. It is difficult to scrape off or otherwise remove such a plaque. The oral cavity becomes dry and rough; When chewing, speaking, and even at rest, patients experience significant discomfort and pain. It should be noted that this disease most often affects men over 30 years of age.
The main cause of the chronic atrophic type is constant injury to the mucous membranes, for example due to wearing a prosthesis. Symptoms of the disease are localized in the affected area. Redness of the mucous membrane occurs (often along the contour of the lesion), plaque forms, pain and burning occur, and the membranes become dry.
Pathological plaque on the tongue
If the white coating on the tongue is caused by an illness, it persists throughout the day. A thin white coating occurs with any ARVI. It disappears as soon as the patient recovers.
Particular attention should be paid to the compaction of plaque. The body of the tongue is not visible through the thick coating. Such plaque is difficult to remove. Thick plaque is considered a sign indicating the severity of the disease.
The color of the coating on the tongue is also important. The more intense the color, the more serious the pathology that caused the plaque. The color of plaque is not only white. A yellowish tint to the plaque may be associated with a malfunction of the gallbladder or pancreas. Gray plaque is possible in case of stomach disease - gastritis, peptic ulcer. In some severe infectious diseases, plaque may acquire a black, bluish or greenish tint.
However, it should be taken into account that the color of plaque can be affected by smoking, drinking and eating.
How does the disease manifest in children?
In children, the disease occurs in an acute form and is accompanied by the appearance of redness and swelling in the oral mucosa. The child sleeps poorly, may have no appetite, and becomes tearful.
The disease can occur in children for the following reasons:
- Weakening of the immune system.
- Infection during breastfeeding.
- Transmission of the fungus during childbirth.
- Infection through household items.
If the disease is not diagnosed and treated in a timely manner, a whitish coating resembling cottage cheese will soon appear in the child’s mouth, and in an advanced stage, ulcers will appear, which are accompanied by bleeding and cause severe pain in children.
Therapy methods
Treatment of candidiasis begins with treatment of the oral cavity. The first procedure is performed by a specialist at the appointment. Antiseptic agents are used to remove plaque. The doctor may then apply an antifungal agent.
The parent should closely monitor the dentist’s actions, since in the future they will have to treat the oral cavity themselves at home. The necessary medications will be prescribed by a specialist. Local antifungal agents are dangerous in case of overdose, especially for children, so you must strictly follow your doctor’s recommendations.
In advanced cases, medications are prescribed in the form of solutions, drops or tablets. There are few drugs available to treat candidiasis in children. Replacing them with adult counterparts is also dangerous. The dosage must be strictly observed.
A mandatory addition to the main therapy is maintaining good hygiene, good sleep, proper nutrition and taking measures to strengthen the immune system (eating healthy foods, taking pharmaceutical vitamins if necessary, walking, etc.).
Diagnostics
To make an accurate diagnosis, a combination of several methods is used - from a simple examination and questioning of the patient for complaints to laboratory methods, such as culture, microscopic examination of biomaterial, analysis of the degree of contamination of the oral cavity with fungal mycelium.
Oral candidiasis is accompanied by a number of characteristic external signs, in particular the formation of plaque, bad breath, ulceration and hyperemia of the mucous membranes. However, laboratory methods make it possible to accurately determine the type of pathogen and exclude the possibility of a secondary infection, which may affect the nature and duration of treatment.
Differential diagnosis is used to separate cases of candidiasis from aphthous stomatitis, leukoplakia, lichen ruber, streptococcal infection and other infectious pathologies of the oral cavity.
What is recommended to rinse your mouth with?
As part of the treatment, various rinses are recommended. As a rule, specialists prescribe solutions for disinfection; they help remove plaque, remove secretions from other areas of the mucous membrane, suppress inflammation, and also heal microtraumas on soft tissues. In such situations, a 2% solution of regular baking soda or a mixture of iodinol and water is often used. It is recommended to repeat rinsing every couple of hours, as well as after waking up and before going to bed. On average, the course lasts about 2 weeks. However, therapy should never be started without the consent of a specialist. Before performing the first procedure, consult your doctor.
Rinsing is prescribed by the attending physician
How to treat oral candidiasis?
Treatment is carried out using local and general, specific and symptomatic remedies. Among the main goals of therapy are the elimination of foci of infection in the oral cavity (sanitation), treatment of diseases that accompany candidiasis and are risk factors, and stimulation of the body's defenses. The total duration of treatment is usually at least 7-10 days.
As a means of local therapy, rinses are used - using solutions of boric acid, soda, sodium tetraborate. For a longer and more effective effect, such products can be used in the form of applications - moistening a cotton swab or bandage with the solution.
Nystatin for oral candidiasis is used to combat the main cause of the disease - a fungal infection. Treatment of candidiasis in the mouth may also include the use of other antimycotic (antifungal) drugs - for example, levorin ointment. The best effect is achieved by using several drugs, alternating them for several days.
Antifungal drugs are also prescribed for systemic therapy - in this case, medications for oral candidiasis and other infections such as Lamisil, Diflucan, Levarin, Nizoral, etc. are taken orally. In the most severe cases of the disease, the treatment regimen includes taking immunomodulatory drugs, as well as the use other agents that have a stimulating effect on the immune system and help strengthen the body’s own defenses.
An equally important task is to protect against additional fungal and bacterial infections that can join the Candida infection and complicate the course of the disease. For this purpose, rinses with antiseptic solutions - fucorcin, iodinol and others.
As an alternative, you can use ASEPTA antiseptic mouth rinse, which contains the active ingredients chlorhexidine and benzydamine. Both of these substances have broad antimicrobial effects. Regular use of ASEPTA rinses also has a pronounced anti-inflammatory effect and helps not only eliminate unpleasant symptoms, but also reduce the risk of complications.
Pathogenesis
Normally, protection against mycotic (fungal) infection is provided by cellular immunity, namely the activity of T-lymphocytes and phagocytes (neutrophils, macrophages and monocytes). Phagocytic cells recognize, engulf and digest fungal cells. With a decrease in immunity and exposure to predisposing factors, phagocytes capture, but are not able to “digest” the fungus of the genus Candida - incomplete phagocytosis develops.
A disruption of the immune response leads to adhesion (attachment) of the fungus to the surface of the mucosa, and local inflammation occurs at this site. Candida then multiplies and penetrates the submucosa and other underlying tissues, disrupting their structure. Due to the presence of specific enzymes, Candida fungi are capable of causing tissue necrosis, which only enhances their adhesive properties and accelerates penetration.
Fungi of the genus Candida differ in their pathogenic activity depending on the species. Candida albicans is considered the most pathogenic, which is capable of changing its phenotype (as conditions for its habitat worsen, it changes from yeast to mold form), receptors and antigens.
Chronic candidiasis infection leads to sensitization (sensitivity) of the body to the fungal antigen and causes the formation of autoantibodies that destroy their own cells - the cells of the human body.
Disease prevention
Preventive measures are aimed at improving the condition of the microflora. These include:
- Proper oral hygiene.
- A thoughtful diet with a high amount of protein foods and reduced consumption of foods containing glucose.
- Quitting smoking and alcoholic beverages.
- Timely examination by the attending dentist for the prevention, diagnosis and treatment of the disease.
- Avoid taking medications, such as antibiotics, without first consulting your doctor.
- If the patient has dentures, then one of the preventive measures will be their regular treatment in a special solution.
Sources:
- The role of anti-inflammatory rinse in the treatment of periodontal diseases (L.Yu. Orekhova, A.A. Leontyev, S.B. Ulitovsky) L.Yu. OREKHOVA, Doctor of Medical Sciences, Prof., Head of Department; A.A. LEONTIEV, dentist; S.B. ULITOVSKY, Doctor of Medical Sciences, Prof. Department of Therapeutic Dentistry of St. Petersburg State Medical University named after. acad. I. P. Pavlova
- Report on clinical trials to determine/confirm the preventive properties of commercially produced personal oral hygiene products: mouth rinse "ASEPTA PARODONTAL" - Solution for irrigator." Doctor of Medical Sciences Professor, Honored Doctor of the Russian Federation, Head. Department of Preventive Dentistry S.B. Ulitovsky, doctor-researcher A.A. Leontiev First St. Petersburg State Medical University named after academician I.P. Pavlova, Department of Preventive Dentistry.
- Study of the clinical effectiveness of treatment and prophylactic agents of the Asepta line in the treatment of inflammatory periodontal diseases (A.I. Grudyanov, I.Yu. Aleksandrovskaya, V.Yu. Korzunina) A.I. GRUDYANOV, Doctor of Medical Sciences, Prof., Head of Department I.Yu. ALEXANDROVSKAYA, Ph.D. V.Yu. KORZUNINA, asp. Department of Periodontology, Central Research Institute of Dentistry and Maxillofacial Surgery, Rosmedtekhnologii, Moscow
Advantages of taking tests at JSC "SZDCM"
- Own laboratory with the latest diagnostic equipment.
- Convenient location of terminals within transport accessibility from anywhere in the city.
- Qualified laboratory technicians and friendly staff.
- Fast analysis and several options for obtaining results. Choose the one that is most convenient for you.
Medical centers and laboratory terminals of the North-Western Center for Evidence-Based Medicine are located in St. Petersburg, Leningrad region, Veliky Novgorod, Okulovka, Kaliningrad and Pskov.
Analyzes
- Bacteriological study for opportunistic pathogenic flora (OPF)
- NC yeasts of the genus Candida: C.albicans, C.krusei, C.glabrata
- Study of the biocenosis of the urogenital tract in women (“Femoflor 13 - screening”)
- Candida albicans
- Mycoses: identification of clinically significant fungi with determination of sensitivity to antimycotic drugs (only for fungi of the genus Candida and Cryptococcus neoformans)
- Specific immunoglobulin E - Candida albicans
go to analyzes